|
Oregon has started providing air conditioners, air purifiers and power banks to help some of its Medicaid recipients cope with soaring heat, smoky skies and other dangers of climate change. It’s a first-in-the-nation experiment that expands a Biden administration strategy to take Medicaid beyond traditional medical care and into the realm of social services. “Climate change is a health-care issue,” Health and Human Services Secretary Xavier Becerra told me, adding that states should be encouraged to experiment with ways to improve people’s health. But Medicaid’s expansion into social services could lead to abuse, especially when government pays for equipment or services that everyone wants, said Sherry Glied, dean of New York University’s graduate school of public service. “The challenge here is that air conditioners are something that both healthy people and people who have your really serious condition benefit from,” Glied said. “Most people have air conditioners for reasons that have nothing to do with their health.” Many states are already spending billions of Medicaid dollars on services like helping homeless people get housing and preparing healthy meals for people with diabetes. But Oregon is the first to spend Medicaid money explicitly on climate-related equipment to help its most vulnerable residents — an estimated 200,000 enrollees. Recipients must meet federal guidelines that categorize them as “facing certain life transitions,” a stringent set of requirements that disqualify most enrollees. For example, a person with an underlying medical condition that could worsen during a heat wave, and who is also at risk for homelessness or has been released from prison in the past year, could receive an air conditioner. But someone with stable housing might not qualify. “Each person is going to be looked at as what they need for their particular circumstance,” said Dave Baden, deputy director for programs and policy at the Oregon Health Authority, which administers the state’s Medicaid program, with about 1.4 million total enrollees. The program, part of a five-year $1.1 billion effort that includes housing and nutrition services, also pays for mini fridges to keep medications cold, portable power supplies to run ventilators and other medical devices during outages, space heaters for winter and air filters to improve air quality during wildfire season. Scientists and public health officials say climate change poses a growing health risk. The federal government’s latest climate assessment projects that more frequent and intense floods, droughts, wildfires, extreme temperatures and storms will cause more deaths, cardiovascular disease from poor air quality and other problems. The mounting health effects disproportionately hit low-income Americans and people of color, who are often covered by Medicaid, the state-federal health insurance program for low-income people. Most of the 102 Oregonians who died during a deadly heat dome that settled over the Pacific Northwest in 2021 “were elderly, isolated and living with low incomes,” a report by the Oregon Health Authority found. This article is not available for syndication due to republishing restrictions. If you have questions about the availability of this or other content for republication, please contact [email protected]. KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about KFF. USE OUR CONTENTThis story can be republished for free (details). from https://ift.tt/kwqdMl9 Check out http://plush-draw15.tumblr.com/
0 Comments
A fresh set from the comfort of your own home? DIY gel nails have been all the rage on social media, but the practice could cause you to develop a life-changing allergy. In a TikTok video, creator @alina.gene describes developing an acrylate allergy from doing gel nails at home. Now, when exposed to acrylates, the creator feels severe pain. The creator warns viewers not to self-apply nail polish that requires a UV light to cure. In later videos, @alina.gene explains that at-home use differs from in-salon use because salon professionals have access to higher-quality chemicals that are less likely to cause reactions and that they also have proper training on how to safely apply the products. “I know I sound real dramatic because an allergy to gel nails or even an allergy to acrylates isn’t going to kill you, but the thing is, in the wrong situation it could prevent you from getting lifesaving medical care,” said @alina.gene in another video. Common medical products contain acrylates, and developing this allergy can cause major issues in obtaining future medical care. We asked an allergist to walk us through this viral video. If you enjoyed this story from the KFF Health News social team, follow us on Instagram @KFFHealthNews. ✍️: KFF Health News Audience Engagement Team KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about KFF. USE OUR CONTENTThis story can be republished for free (details). from https://ift.tt/RvFEZMP Check out http://plush-draw15.tumblr.com/ “Congress prohibits the NIH from researching the cause of mass shootings.” Robert F. Kennedy Jr. in an April 21 post on X The National Institutes of Health is the federal government’s main agency for supporting medical research. Is it barred from researching mass shootings? That’s what presidential candidate Robert F. Kennedy Jr. said recently. Kennedy, whose statements about conspiracy theories earned him PolitiFact’s 2023 “Lie of the Year,” is running as an independent third-party candidate against President Joe Biden, the presumptive Democratic candidate, and the presumptive Republican nominee, former President Donald Trump. On April 21 on X, Kennedy flagged his recent interview with conservative commentator Glenn Beck, which touched on gun policy. Kennedy summarized his gun policy views in the post, writing, “The National Institutes of Health refuses to investigate the mystery; in fact, Congress prohibits the NIH from researching the cause of mass shootings. Under my administration, that rule ends — and our kids’ safety becomes a top priority.” But this information is outdated. In 1996, Congress passed the “Dickey Amendment,” an appropriations bill provision that federal officials widely interpreted as barring federally funded research related to gun violence (though some observers say this was a misinterpretation). Congress in 2018 clarified that the provision didn’t bar federally funded gun-related research, and funding for such efforts has been flowing since 2020. Kennedy’s campaign did not provide evidence to support his statement. What Was the Dickey Amendment? After criticizing some federally funded research papers on firearms in the mid-1990s, pro-gun advocates, including the National Rifle Association, lobbied to halt federal government funding for gun violence research. In 1996, Congress approved appropriations bill language saying that “none of the funds made available for injury prevention and control at the Centers for Disease Control and Prevention may be used to advocate or promote gun control.” The language was named for one of its backers, Rep. Jay Dickey (R-Ark). But the Dickey Amendment, as written, did not ban all gun-related research outright. “Any honest research that was not rigged to produce results that helped promote gun control could be funded by CDC,” said Gary Kleck, a Florida State University criminologist. But CDC officials, experts said, interpreted the Dickey Amendment as banning all gun-related research funding. This perception meant the amendment “had a chilling effect on funding for gun research,” said Allen Rostron, a University of Missouri-Kansas City law professor who has written about the amendment. Federal agencies “did not want to take a chance on funding research that might be seen as violating the restriction” and so “essentially were not funding research on gun violence.” Also, the Dickey Amendment targeted only the CDC, not all other federal agencies. Congress expanded the restriction to cover NIH-funded research in 2011. Although the Dickey Amendment didn’t bar gun-related research, federal decision-makers acted as though it did by not pursuing such research. Moving Past the Dickey Amendment Over time, critics of the gun industry made an issue of the Dickey Amendment and gathered congressional support to clarify the amendment. In 2018, lawmakers approved language that said the amendment wasn’t a blanket ban on federally funded gun violence research. By 2020, federal research grants on firearms began to be issued again, starting with $25 million to be split between the CDC and NIH. By now, the CDC and NIH are funding a “large portfolio” of firearm violence-related research, said Daniel Webster, a professor at the Johns Hopkins Bloomberg School of Public Health. Also, the Justice Department’s National Institute of Justice has funded the largest study of mass shootings to date, Webster said, and is seeking applications for studies of mass shootings. Our Ruling Kennedy said, “Congress prohibits the NIH from researching the cause of mass shootings.” Although the Dickey Amendment, a provision of appropriations law supported by the gun industry, didn’t prohibit all federally supported, gun-related research from 1996 to 2018, decision-makers acted as though it did. However, in 2018, Congress clarified the provision’s language. And since 2020, CDC, NIH, and other federal agencies have funded millions of dollars in gun-related research, including studies on mass shootings. We rate Kennedy’s statement False. Our SourcesRobert F. Kennedy Jr. post on X, April 21, 2024 National Institutes of Health, “NIH Awards Additional Research and Training Grants to Support Firearm Injury and Mortality Prevention Science,” Sept. 20, 2023 National Institute of Justice, “Public Mass Shootings: Database Amasses Details of a Half Century of U.S. Mass Shootings with Firearms, Generating Psychosocial Histories,” Feb. 3, 2022 National Institute of Justice, “NIJ FY24 Research and Evaluation on Firearm Violence and Mass Shootings,” Feb. 5, 2024 Centers for Disease Control and Prevention, “Funded Research,” accessed April 22, 2024 American Psychological Association, “A Thaw in the Freeze on Federal Funding for Gun Violence and Injury Prevention Research,” April 1, 2021 Allen Rostron, “The Dickey Amendment on Federal Funding for Research on Gun Violence: A Legal Dissection” (American Journal of Public Health), July 2018 Email interview with Gary Kleck, a Florida State University criminologist, April 22, 2024 Email interview with Daniel W. Webster, professor at the Johns Hopkins Bloomberg School of Public Health, April 22, 2024 Email interview with Jaclyn Schildkraut, executive director of the Regional Gun Violence Research Consortium at the Rockefeller Institute of Government, April 22, 2024 Email interview with Mike Lawlor, University of New Haven criminologist, April 22, 2024 Email interview with Allen Rostron, University of Missouri-Kansas City law professor, April 22, 2024 KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about KFF. USE OUR CONTENTThis story can be republished for free (details). from https://ift.tt/kugilG6 Check out http://plush-draw15.tumblr.com/ SACRAMENTO, Calif. — Families of people with intellectual and developmental disabilities say Gov. Gavin Newsom is reneging on a scheduled raise for the workers who care for their loved ones, and advocates warn of potential lawsuits if disability services become harder to get. Citing California’s budget deficit, the Democratic governor wants to save around $613 million in state funds by delaying pay increases for a year for about 150,000 disability care workers. The state will forgo an additional $408 million in Medicaid reimbursements, reducing funding by over $1 billion. Some lawmakers say this decision will increase staff turnover and vacancies, leaving thousands of children and adults with disabilities without critical services at home and in residential facilities. Disability advocates warn it could violate the Lanterman Act, California’s landmark law that says the state must provide services and resources to people with disabilities and their families. Newsom is “breaking a promise,” said Felisa Strickland, 60, who has been searching for more than a year for a day program for her 23-year-old daughter, Lily, who has autism and cerebral palsy. “It’s creating a lot of physical and mental health problems for people, and it’s a lot of undue stress on aging parent caregivers like myself.” Disability care workers, known as direct support professionals, provide daily, hands-on caregiving to help children and adults with intellectual and developmental disabilities, such as autism, cerebral palsy, and epilepsy, remain independent and integrated into their communities. In California, more than 400,000 people with disabilities need accommodation, and this population, along with seniors, is increasing. It’s not clear how big the worker shortage is because the state hasn’t released workforce data. As the demand for these workers grows generally, experts predict a shortage of between 600,000 and 3.2 million direct care workers by 2030. Advocates say California pays most providers from $16 to $20 an hour, which meets the state’s minimum wage but falls short of what some economists consider a living wage. In 2021, the state committed to raising wages after identifying a $1.8 billion gap between the rates received by nonprofits that contract with the state to provide care and the rates deemed adequate. Thus far, the state has provided around half that total, most of which has gone to raising wages and benefits. Workers had been expecting one more increase, of $2-$4 an hour, in July, until Newsom proposed a delay. Also, nonprofits say California has made it harder to compete for workers after raising wages in other service and health industries. Newsom approved a $20 minimum wage for fast-food workers that went into effect in April and he struck a deal last year with unions and hospitals to begin raising health care workers’ wages to a minimum of $25 an hour. Ricardo Zegri said Taco Bell would pay him more than the $19 an hour he makes as a disability care worker in a supervisory position. “Every paycheck, it’s a discussion at home about what bills we need to prioritize and whether it’s time to start looking for work that pays more,” said Zegri, who works a second job as a musician in the San Francisco Bay Area.  
Newsom wants to preserve key health initiatives, including the state expansion of Medi-Cal to low-income immigrants regardless of legal status, and CalAIM, an ambitious $12 billion experiment to transform Medi-Cal into both a health insurer and a social services provider. However, the rate delay for providing disability care is the largest savings in the Health and Human Services budget as Newsom and legislative leaders look to cuts, delays, and shifts in funding to close a deficit estimated between $38 billion and $73 billion. Dozens of legislators from both parties are asking Newsom and legislative leaders to preserve the increase. Assembly member Stephanie Nguyen, a Democrat from Elk Grove, signed a letter supporting the raise. Although lawmakers are negotiating with the administration, she said reversing the decision to delay the pay boost is unlikely. Everybody “has to take a hit somewhere,” Nguyen said. Krystyne McComb, a spokesperson for the Department of Developmental Services, said even though the state would lose federal matching funds this year, it would resume drawing funds when the state reinstates the plan in 2025. The department did not respond to questions about how it plans to retain workers and fill vacancies. Newsom’s proposal risks a collapse of the disability service system, which would violate the Lanterman Act and make the state vulnerable to lawsuits, said Jordan Lindsey, executive director of the Arc of California, a statewide disability rights advocacy organization. Families say the state has already fallen short on services they need. Strickland quit her job to care for Lily, the Santa Barbara mother said. “It’s not reasonable to expect someone to care for somebody else 24 hours a day, seven days a week,” she said. Lily graduated from high school and in 2022 completed a program that prepares youth with disabilities to transition into adult life. She had been looking forward to joining a day program to make new friends but has yet to find a spot. And due to a shortage of workers, Lily receives only four hours a week at home with a provider, who is paid around $16 an hour. When Lily hangs out with the provider, her demeanor changes to the happy person she used to be, Strickland said. “The system is already in crisis,” she said. “There are tons and tons of people that are sitting at home because there’s nowhere for them to go.” KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about KFF. USE OUR CONTENTThis story can be republished for free (details). from https://ift.tt/X6gzhJ8 Check out http://plush-draw15.tumblr.com/ The World Health Organization has issued a report that transforms how the world understands respiratory infections like covid-19, influenza, and measles. Motivated by grave missteps in the pandemic, the WHO convened about 50 experts in virology, epidemiology, aerosol science, and bioengineering, among other specialties, who spent two years poring through the evidence on how airborne viruses and bacteria spread. However, the WHO report stops short of prescribing actions that governments, hospitals, and the public should take in response. It remains to be seen how the Centers for Disease Control and Prevention will act on this information in its own guidance for infection control in health care settings. The WHO concluded that airborne transmission occurs as sick people exhale pathogens that remain suspended in the air, contained in tiny particles of saliva and mucus that are inhaled by others. While it may seem obvious, and some researchers have pushed for this acknowledgment for more than a decade, an alternative dogma persisted — which kept health authorities from saying that covid was airborne for many months into the pandemic. Specifically, they relied on a traditional notion that respiratory viruses spread mainly through droplets spewed out of an infected person’s nose or mouth. These droplets infect others by landing directly in their mouth, nose, or eyes — or they get carried into these orifices on droplet-contaminated fingers. Although these routes of transmission still happen, particularly among young children, experts have concluded that many respiratory infections spread as people simply breathe in virus-laden air. “This is a complete U-turn,” said Julian Tang, a clinical virologist at the University of Leicester in the United Kingdom, who advised the WHO on the report. He also helped the agency create an online tool to assess the risk of airborne transmission indoors. Peg Seminario, an occupational health and safety specialist in Bethesda, Maryland, welcomed the shift after years of resistance from health authorities. “The dogma that droplets are a major mode of transmission is the ‘flat Earth’ position now,” she said. “Hurray! We are finally recognizing that the world is round.” The change puts fresh emphasis on the need to improve ventilation indoors and stockpile quality face masks before the next airborne disease explodes. Far from a remote possibility, measles is on the rise this year and the H5N1 bird flu is spreading among cattle in several states. Scientists worry that as the H5N1 virus spends more time in mammals, it could evolve to more easily infect people and spread among them through the air. Traditional beliefs on droplet transmission help explain why the WHO and the CDC focused so acutely on hand-washing and surface-cleaning at the beginning of the pandemic. Such advice overwhelmed recommendations for N95 masks that filter out most virus-laden particles suspended in the air. Employers denied many health care workers access to N95s, insisting that only those routinely working within feet of covid patients needed them. More than 3,600 health care workers died in the first year of the pandemic, many due to a lack of protection. However, a committee advising the CDC appears poised to brush aside the updated science when it comes to its pending guidance on health care facilities. Lisa Brosseau, an aerosol expert and a consultant at the Center for Infectious Disease Research and Policy in Minnesota, warns of a repeat of 2020 if that happens. “The rubber hits the road when you make decisions on how to protect people,” Brosseau said. “Aerosol scientists may see this report as a big win because they think everything will now follow from the science. But that’s not how this works and there are still major barriers.” Money is one. If a respiratory disease spreads through inhalation, it means that people can lower their risk of infection indoors through sometimes costly methods to clean the air, such as mechanical ventilation and using air purifiers, and wearing an N95 mask. The CDC has so far been reluctant to press for such measures, as it updates foundational guidelines on curbing airborne infections in hospitals, nursing homes, prisons, and other facilities that provide health care. This year, a committee advising the CDC released a draft guidance that differs significantly from the WHO report. Whereas the WHO report doesn’t characterize airborne viruses and bacteria as traveling short distances or long, the CDC draft maintains those traditional categories. It prescribes looser-fitting surgical masks rather than N95s for pathogens that “spread predominantly over short distances.” Surgical masks block far fewer airborne virus particles than N95s, which cost roughly 10 times as much. Researchers and health care workers have been outraged about the committee’s draft, filing letters and petitions to the CDC. They say it gets the science wrong and endangers health. “A separation between short- and long-range distance is totally artificial,” Tang said. Airborne viruses travel much like cigarette smoke, he explained. The scent will be strongest beside a smoker, but those farther away will inhale more and more smoke if they remain in the room, especially when there’s no ventilation. Likewise, people open windows when they burn toast so that smoke dissipates before filling the kitchen and setting off an alarm. “You think viruses stop after 3 feet and drop to the ground?” Tang said of the classical notion of distance. “That is absurd.”  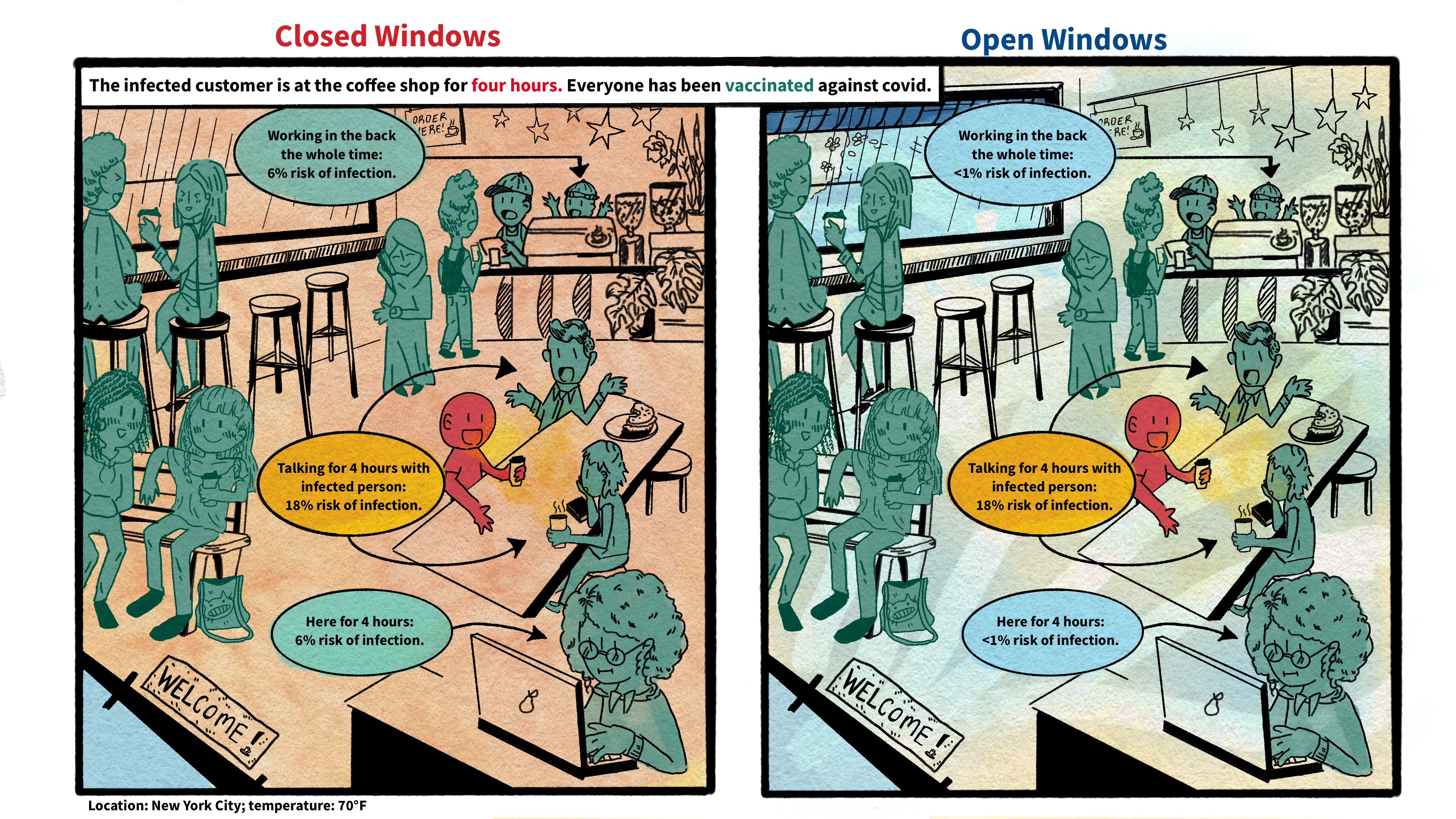
The CDC’s advisory committee is comprised primarily of infection control researchers at large hospital systems, while the WHO consulted a diverse group of scientists looking at many different types of studies. For example, one analysis examined the puff clouds expelled by singers, and musicians playing clarinets, French horns, saxophones, and trumpets. Another reviewed 16 investigations into covid outbreaks at restaurants, a gym, a food processing factory, and other venues, finding that insufficient ventilation probably made them worse than they would otherwise be. In response to the outcry, the CDC returned the draft to its committee for review, asking it to reconsider its advice. Meetings from an expanded working group have since been held privately. But the National Nurses United union obtained notes of the conversations through a public records request to the agency. The records suggest a push for more lax protection. “It may be difficult as far as compliance is concerned to not have surgical masks as an option,” said one unidentified member, according to notes from the committee’s March 14 discussion. Another warned that “supply and compliance would be difficult.” The nurses’ union, far from echoing such concerns, wrote on its website, “The Work Group has prioritized employer costs and profits (often under the umbrella of ‘feasibility’ and ‘flexibility’) over robust protections.” Jane Thomason, the union’s lead industrial hygienist, said the meeting records suggest the CDC group is working backward, molding its definitions of airborne transmission to fit the outcome it prefers. Tang expects resistance to the WHO report. “Infection control people who have built their careers on this will object,” he said. “It takes a long time to change people’s way of thinking.” The CDC declined to comment on how the WHO’s shift might influence its final policies on infection control in health facilities, which might not be completed this year. Creating policies to protect people from inhaling airborne viruses is complicated by the number of factors that influence how they spread indoors, such as ventilation, temperature, and the size of the space. Adding to the complexity, policymakers must weigh the toll of various ailments, ranging from covid to colds to tuberculosis, against the burden of protection. And tolls often depend on context, such as whether an outbreak happens in a school or a cancer ward. “What is the level of mortality that people will accept without precautions?” Tang said. “That’s another question.” KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about KFF. USE OUR CONTENTThis story can be republished for free (details). from https://ift.tt/frgq9TP Check out http://plush-draw15.tumblr.com/ La OMS confirma cómo se propagan los virus por el aire. Los CDC tal vez miren para otro lado5/1/2024 La Organización Mundial de la Salud (OMS) ha emitido un informe que transforma la manera en que el mundo comprende infecciones respiratorias como covid-19, la gripe y el sarampión. Motivada por graves errores durante la pandemia, la OMS convocó a unos 50 expertos en virología, epidemiología, ciencia de aerosoles e ingeniería biológica, entre otras especialidades, que pasaron dos años revisando evidencia sobre cómo se propagan los virus y bacterias por el aire. El informe de la OMS no recomienda acciones a los gobiernos, hospitales o al público en general. Queda por ver si los Centros para el Control y Prevención de Enfermedades (CDC) utilizarán esta información en su propia orientación sobre el control de infecciones en entornos de atención médica. La OMS concluyó que la transmisión aérea ocurre cuando las personas enfermas exhalan patógenos que quedan suspendidos en el aire, contenidos en pequeñas partículas de saliva y moco que, a su vez, son inhaladas por otros. Aunque pueda parecer obvio, y algunos investigadores han abogado por este reconocimiento durante más de una década, el que perduró es un dogma alternativo que impidió a las autoridades sanitarias decir que el covid se transmitía por vía aérea hasta muchos meses entrada la pandemia. Específicamente, se basaron en la noción tradicional de que los virus respiratorios se propagan principalmente a través de gotas expulsadas por la nariz o la boca de una persona infectada. Estas gotas infectan a otros al caer directamente en su boca, nariz u ojos, o entran en estos orificios por los dedos contaminados con estas gotas. Aunque estas vías de transmisión siguen ocurriendo, especialmente entre niños pequeños, expertos han concluido que muchas infecciones respiratorias se propagan simplemente al inhalar aire contaminado con virus. “Esto es un cambio radical”, dijo Julian Tang, virólogo clínico de la Universidad de Leicester en el Reino Unido, quien asesoró a la OMS para el informe. También ayudó a la agencia a crear una herramienta en línea para evaluar el riesgo de transmisión aérea en interiores. Peg Seminario, especialista en salud y seguridad ocupacional en Bethesda, Maryland, aplaudió el cambio después que las autoridades sanitarias se resistieran por años. “El dogma de que las gotas son una forma principal de transmisión es ahora la posición de la ‘Tierra plana'”, dijo. “¡Viva! Finalmente estamos reconociendo que la Tierra es redonda”. El cambio pone un nuevo énfasis en la necesidad de mejorar la ventilación en interiores y almacenar máscaras de calidad antes que se desate la próxima enfermedad transmitida por vía aérea. Lejos de ser una posibilidad remota, el sarampión está en aumento este año y la gripe aviar H5N1 se está propagando entre el ganado en varios estados. Los científicos temen que a medida que el virus H5N1 pase más tiempo en mamíferos, podría evolucionar para infectar más fácilmente a las personas y propagarse entre ellas por el aire. Las creencias tradicionales sobre la transmisión por gotas ayudan a explicar por qué la OMS y los CDC se centraron tanto en lavarse las manos y en limpiar las superficies al comienzo de la pandemia. Estos consejos eclipsaron las recomendaciones para el uso de máscaras N95 que filtran la mayoría de las partículas de virus suspendidas en el aire. Los empleadores negaron a muchos trabajadores de salud el acceso a las N95, insistiendo en que solo aquellos que trabajaban rutinariamente a pocos metros de pacientes con covid las necesitaban. Más de 3,600 trabajadores de salud murieron en el primer año de la pandemia, muchos debido a la falta de protección. Sin embargo, un comité asesor de los CDC parecen estar dispuesto a ignorar la actualización científica cuando se trata de su propia orientación pendiente sobre las instalaciones de atención médica. Lisa Brosseau, experta en aerosoles y consultora del Centro de Investigación y Política de Enfermedades Infecciosas en Minnesota, advierte sobre volver a vivir el 2020 si eso sucede. “El momento de la verdad llega cuando se toman decisiones sobre cómo proteger a las personas”, dijo Brosseau. “Los científicos de aerosoles pueden ver este informe como una gran victoria porque piensan que a partir de ahora todo seguirá a la ciencia. Pero esto no funciona así y todavía hay barreras importantes”. El dinero es una de ellas. Si una enfermedad respiratoria se propaga por inhalación, significa que las personas pueden reducir su riesgo de infección en interiores a través de métodos a veces costosos para limpiar el aire, como la ventilación mecánica o los purificadores de aire, y usando una máscara N95. Hasta ahora, los CDC han sido reacios a presionar por tales acciones, mientras actualiza las directrices fundamentales para frenar las infecciones transmitidas por el aire en hospitales, hogares de adultos mayores, prisiones y otras instalaciones que brindan atención médica. Este año, un comité asesor de los CDC publicó el borrador de una guía que difiere significativamente del informe de la OMS. Mientras que el informe de la OMS no caracteriza a los virus y bacterias transmitidos por vía aérea como “viajeros” de distancias cortas o largas, el borrador de los CDC mantiene esas categorías tradicionales. Recomienda máscaras quirúrgicas menos ajustadas, en lugar de las N95 para patógenos que “se propagan predominantemente por distancias cortas”. Las máscaras quirúrgicas bloquean muchas menos partículas de virus en el aire que las N95, que cuestan aproximadamente 10 veces más. Los investigadores y trabajadores de salud han reaccionado con indignación al borrador del comité, y han enviado cartas y peticiones a los CDC. Dicen que tergiversa la ciencia y que pone en peligro la salud. “Una separación entre distancias cortas y largas es totalmente artificial”, dijo Tang. Los virus transmitidos por aire viajan de manera similar al humo del cigarrillo, explicó. El olor será más fuerte junto a un fumador, pero los que están más lejos inhalarán más y más humo si permanecen en la habitación, especialmente cuando no hay ventilación. De la misma manera, las personas abren ventanas cuando queman tostadas para que el humo se disipe antes de llenar la cocina y activar una alarma. “¿Creen que los virus se detienen después de 3 pies y caen al suelo?”, dijo Tang sobre la noción clásica de distancia. “Eso es absurdo”. El comité asesor de los CDC está compuesto principalmente por investigadores de control de infecciones en grandes sistemas hospitalarios, mientras que la OMS consultó a un grupo diverso de científicos que examinaron muchos tipos diferentes de estudios. Por ejemplo, uno de los análisis de la OMS examinó las nubes de vapor expulsadas por cantantes y músicos que tocaban clarinetes, trombones, saxofones y trompetas. Otro revisó 16 investigaciones sobre brotes de covid en restaurantes, un gimnasio, una fábrica de procesamiento de alimentos y otros lugares, encontrando que una ventilación insuficiente probablemente empeoró el problema sanitario. En respuesta a la protesta, los CDC devolvieron el borrador a su comité para su revisión, pidiéndole que reconsiderara sus consejos. Desde entonces, se han realizado reuniones privadas con un grupo de trabajo ampliado. Pero el sindicato National Nurses United obtuvo notas de las conversaciones a través de una solicitud de registros públicos a la agencia. Los registros sugieren una presión para una protección más relajada. “Puede ser difícil en cuanto a la conformidad no tener las mascarillas quirúrgicas como una opción”, dijo un miembro no identificado, según las notas de la discusión del comité del 14 de marzo. Otro advirtió que “el suministro y el cumplimiento serían difíciles”. El sindicato de enfermeras escribió en su sitio web: “El Grupo de Trabajo ha priorizado los costos y ganancias del empleador (a menudo bajo el paraguas de ‘viabilidad’ y ‘flexibilidad’) por sobre las protecciones sólidas”. Jane Thomason, higienista industrial principal del sindicato, dijo que los registros de la reunión sugieren que el grupo de los CDC está trabajando al revés: moldeando sus definiciones de transmisión aérea para que se ajusten al resultado que prefiere. Tang espera resistencia al informe de la OMS. “Las personas de control de infecciones que han construido sus carreras en esto se opondrán”, dijo. “Se necesita mucho tiempo para cambiar la forma de pensar de las personas”. Los CDC se negaron a hacer comentarios sobre cómo el cambio de la OMS podría influir en sus políticas finales sobre el control de infecciones en instalaciones de salud, normas que podrían no completarse este año. Formular políticas para proteger a las personas de inhalar virus transmitidos por el aire es algo complejo por la cantidad de factores que influyen en cómo se propagan en interiores, como la ventilación, la temperatura y el tamaño del espacio. Agrega complejidad que los responsables de formularlas deben sopesar el costo de varias dolencias, desde el covid hasta los resfriados y la tuberculosis, contra la carga de la protección. Y los costos a menudo dependen del contexto: si un brote ocurre en una escuela o en una sala oncológica. “¿Cuál es el nivel de mortalidad que las personas aceptarán sin precauciones?”, dijo Tang. “Esa es otra pregunta”. KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about KFF. USE OUR CONTENTThis story can be republished for free (details). from https://ift.tt/X5wYiyM Check out http://plush-draw15.tumblr.com/ Oregon is shipping air conditioners, air purifiers, and power banks to some of its most vulnerable residents, a first-in-the-nation experiment to use Medicaid money to prevent the potentially deadly health effects of extreme heat, wildfire smoke, and other climate-related disasters. The equipment, which started going out in March, expands a Biden administration strategy to move Medicaid beyond traditional medical care and into the realm of social services. At least 20 states, including California, Massachusetts, and Washington, already direct billions of Medicaid dollars into programs such as helping homeless people get housing and preparing healthy meals for people with diabetes, according to KFF. Oregon is the first to use Medicaid money explicitly for climate-related costs, part of its five-year, $1.1 billion effort to address social needs, which also includes housing and nutrition benefits. State and federal health officials hope to show that taxpayer money and lives can be saved when investments are made before disaster strikes. “Climate change is a health care issue,” so helping Oregon’s poorest and sickest residents prepare for potentially dangerous heat, drought, and other extreme weather makes sense, said Health and Human Services Secretary Xavier Becerra on a visit to Sacramento, California, in early April. Becerra said the Biden administration wants states to experiment with how best to improve patient health, whether by keeping someone housed instead of homeless, or reducing their exposure to heat with an air conditioner. But Medicaid’s expansion into social services may duplicate existing housing and nutrition programs offered by other federal agencies, while some needy Americans can’t get essential medical care, said Gary Alexander, director of the Medicaid and Health Safety Net Reform Initiative at the Paragon Health Institute. “There are 600,000 or 700,000 intellectually disabled people in the United States waiting for Medicaid services. They’re on a waitlist,” said Alexander, who oversaw state health agencies in Pennsylvania and Rhode Island. “Meanwhile Medicaid has money for housing and food and air conditioners for recipients. Seems to me that we should serve the intellectually disabled first before we get into all of these new areas.” Scientists and public health officials say climate change poses a growing health risk. More frequent and intense floods, droughts, wildfires, extreme temperatures, and storms cause more deaths, cardiovascular disease from poor air quality, and other problems, according to the federal government’s Fifth National Climate Assessment. The mounting health effects disproportionately hit low-income Americans and people of color, who are often covered by Medicaid, the state-federal health insurance program for low-income people. Most of the 102 Oregonians who died during the deadly heat dome that settled over the Pacific Northwest in 2021 “were elderly, isolated and living with low incomes,” according to a report by the Oregon Health Authority, which administers the state’s Medicaid program, with about 1.4 million enrollees. The OHA’s analysis of urgent care and emergency room use from May through September of 2021 and 2022 found that 60% of heat-related illness visits were from residents of areas with a median household income below $50,000. “In the last 10-plus years, the amount of fires and smoke events and excessive heat events that we’ve had has shown the disproportionate impact of those events on those with lower incomes,” said Dave Baden, the OHA’s deputy director for programs and policy. And, because dangerously high temperatures aren’t common in Oregon, many residents don’t have air conditioning in their homes. Traditionally, states hit by natural disasters and public health emergencies have asked the federal government for permission to spend Medicaid dollars on back-up power, air filters, and other equipment to help victims recover. But those requests came after the fact, following federal emergency declarations. Oregon wants to be proactive and pay for equipment that will help an estimated 200,000 residents manage their health at home before extreme weather or climate-related disaster hits, Baden said. In addition to air conditioning units, the program will pay for mini fridges to keep medications cold, portable power supplies to run ventilators and other medical devices during outages, space heaters for winter, and air filters to improve air quality during wildfire season. In March, the Oregon Health Plan, the state’s Medicaid program, began asking health insurers to find patients who might need help coping with extreme weather. Recipients must meet federal guidelines that categorize them as “facing certain life transitions,” a stringent set of requirements that disqualify most enrollees. For example, a person with an underlying medical condition that could worsen during a heat wave, and who is also at risk for homelessness or has been released from prison in the past year, could receive an air conditioner. But someone with stable housing might not qualify. “You could be in a housing complex, and your neighbor qualified for an air conditioner and you didn’t,” Baden said. At the offices of insurer AllCare Health in Grants Pass, Oregon, air conditioners, air filters, and mini fridges were piled in three rooms in mid-April, ready to be handed over to Medicaid patients. The health plan provided equipment to 19 households in March. The idea is to get the supplies into people’s homes before the summer fire season engulfs the valley in smoke. Health plans don’t want to find themselves “fighting the masses” at Home Depot when the skies are already smoky or the heat is unbearable, said Josh Balloch, AllCare’s vice president of health policy. “We’re competing against everybody else, and you can’t find a fan on a hot day,” he said. Oregon and some other states have already used Medicaid money to buy air conditioners, air purifiers, and other goods for enrollees, but not under the category of climate change. For example, California offers air purifiers to help asthma patients and New York just won federal approval to provide air conditioners to asthma patients. Baden said Oregon health officials will evaluate whether sending air conditioners and other equipment to patients saves money by looking at their claim records in the coming years. If Oregon can help enrollees avoid a costly trip to the doctor or the ER after extreme weather, other state Medicaid programs may ask the federal government if they can adopt the benefit. Many states haven’t yet used Medicaid money for climate change because it affects people and regions differently, said Paul Shattuck, a senior fellow at Mathematica, a research organization that has surveyed state Medicaid directors on the issue. “The health risks of climate change are everywhere, but the nature of risk exposure is completely different in every state,” Shattuck said. “It’s been challenging for Medicaid to get momentum because each state is left to their own devices to figure out what to do.” A California state lawmaker last year introduced legislation that would have required Medi-Cal, the state’s Medicaid program, to add a climate benefit under its existing social services expansion. The program would have been similar to Oregon’s, but AB 586, by Assembly member Lisa Calderon, died in the Assembly Appropriations Committee, which questioned in a staff analysis whether “climate change remediation supports can be defined as cost-effective.” The cost savings are clear to Kaiser Permanente. After the 2021 heat wave, it sent air conditioners to 81 patients in Oregon and southwest Washington whose health conditions might get worse in extreme heat, said Catherine Potter, community health consultant at the health system. The following year, Kaiser Permanente estimated it had prevented $42,000 in heat-related ER visits and $400,000 in hospital admissions, she said. “We didn’t used to have extreme heat like this, and we do now,” said Potter, who has lived in the temperate Portland area for 30 years. “If we can prevent these adverse impacts, we should be preventing them especially for people that are going to be most affected.” This article was produced by KFF Health News, which publishes California Healthline, an editorially independent service of the California Health Care Foundation. KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about KFF. USE OUR CONTENTThis story can be republished for free (details). from https://ift.tt/sdWhmAE Check out http://plush-draw15.tumblr.com/ The Department of Veterans Affairs has long given Vietnam veterans disability compensation for illness connected to Agent Orange, widely used to defoliate Southeast Asian battlefields during the U.S. war. Less well known: The powerful herbicide combination was also routinely used to kill weeds at domestic military bases. Those exposed to the chemicals at the bases are still waiting for the same benefits and, in some cases, are hitting a familiar obstacle — government opacity. In February, VA proposed a rule that for the first time would allow compensation for Agent Orange exposure at 17 U.S. bases in a dozen states where the herbicide was tested, used or stored. But the list excludes about four dozen bases where Pat Elder, an activist and director of the environmental advocacy group Military Poisons, says he’s documented the use or storage of Agent Orange. Among them is Fort Ord, a former Army base in Monterey County, Calif. Documents gathered by Elder and others, including a report by an Army agronomist, a journal article and records related to hazardous material cleanups, establish the use of Agent Orange at the facility. “In training areas, such as Fort Ord, where poison oak has been extremely troublesome to military personnel, a well-organized chemical war has been waged against this woody plant pest,” reads a 1956 article in the journal the Military Engineer. “Until Fort Ord is recognized by VA as a presumptive site, it’s probably going to be a long, difficult struggle to get some kind of compensation,” said Mike Duris, a veteran who trained at the base and was later diagnosed with prostate cancer. VA considers prostate cancer a “presumptive condition” for Agent Orange disability compensation, meaning the agency presumes the illness is linked to exposure to the chemical. It acknowledges that those who served in specific locations were likely exposed and their illnesses are tied to military service. The designation expedites affected veterans’ disability claims. Agent Orange is a 50-50 mixture of two chemicals known as 2,4-D and 2,4,5-T. Herbicides with the same chemical structure, although slightly modified, were widely available in the 1950s and ‘60s, sold commercially and used on practically every base in the United States, said Gerson Smoger, a lawyer who argued before the Supreme Court for Vietnam veterans to have the right to sue Agent Orange manufacturers. 2,4,5-T contains the dioxin TCDD, a known carcinogen linked to a number of cancers, chronic conditions and birth defects. The Environmental Protection Agency banned the use of 2,4,5-T in the United States in 1979. VA says it based its proposed rule on information provided by the Defense Department, and that the Pentagon’s review “found no documentation of herbicide use, testing or storage at Fort Ord.” Patricia Kime contributed reporting. This article is not available for syndication due to republishing restrictions. If you have questions about the availability of this or other content for republication, please contact [email protected]. KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about KFF. USE OUR CONTENTThis story can be republished for free (details). from https://ift.tt/eArxn45 Check out http://plush-draw15.tumblr.com/ MEMPHIS, Tenn. — For many years, Rose Sims had no idea what was going on inside a nondescript brick building on Florida Street a couple of miles from her modest one-story home on the southwestern side of town. Like other residents, she got an unwelcome surprise in October 2022 at a public forum held by the Environmental Protection Agency at the historic Monumental Baptist Church, known for its role in the civil rights movement. The EPA notified the predominantly Black community that Sterilization Services of Tennessee —which began operations in the brick building in the 1970s — had been emitting unacceptably high levels of ethylene oxide, a toxic gas commonly used to disinfect medical devices. Airborne emissions of the colorless gas can increase the risk of certain medical conditions, including breast cancer. Sims, who is 59 and Black, said she developed breast cancer in 2019, despite having no family history of it, and she suspects ethylene oxide was a contributing factor. “I used to be outside a lot. I was in good health. All of a sudden, I got breast cancer,” she said. Local advocates say the emissions are part of a pattern of environmental racism. The term is often applied when areas populated primarily by racial and ethnic minorities and members of low-socioeconomic backgrounds, like southwest Memphis, are burdened with a disproportionate amount of health hazards. The drivers of environmental racism include the promise of tax breaks for industry to locate a facility in a heavily minority community, said Malini Ranganathan, an urban geographer at American University in Washington, D.C. The cheaper cost of land also is a factor, as is the concept of NIMBY — or “not in my backyard” — in which power brokers steer possible polluters to poorer areas of cities. A manager at Sterilization Services’ corporate office in Richmond, Virginia, declined to answer questions from KFF Health News. An attorney with Leitner, Williams, Dooley & Napolitan, a law firm that represents the company, also declined to comment. Sterilization Services, in a legal filing asking for an ethylene oxide-related lawsuit to be dismissed, said the use of the gas, which sterilizes about half the medical devices in the U.S., is highly regulated to ensure public safety. Besides southwest Memphis, there are nearly two dozen locales, mostly small cities — from Athens, Texas, to Groveland, Florida, and Ardmore, Oklahoma — where the EPA said in 2022 that plants sterilizing medical devices emit the gas at unusually high levels, potentially increasing a person’s risk of developing cancer. The pollution issue is so bad in southwest Memphis that even though Sterilization Services planned to close shop by April 30, local community leaders have been hesitant to celebrate. In a letter last year to a local Congress member, the company said it has always complied with federal, state, and local regulations. The reason for its closure, it said, was a problem with renewing the building lease. But many residents see it as just one small win in a bigger battle over environmental safety in the neighborhood. “It’s still a cesspool of pollution,’’ said Yolonda Spinks, of the environmental advocacy organization Memphis Community Against Pollution, about a host of hazards the community faces. The air in this part of the city has long been considered dangerous. An oil refinery spews a steady plume of white smoke. A coal plant has leaked ash into the ground and the groundwater. The coal plant was replaced by a natural gas power plant, and now the Tennessee Valley Authority, which provides electricity for local power companies, plans to build a new gas plant there. A continual stream of heavy trucks chug along nearby highways and roads. Other transportation sources of air pollution include the Memphis International Airport and barge traffic on the nearby Mississippi River. Lead contamination is also a concern, not just in drinking water but in the soil from now-closed lead smelters, said Chunrong Jia, a professor of environmental health at the University of Memphis. Almost all the heavy industry in Shelby County — and the associated pollutants — are located in southwest Memphis, Jia added. Sources of pollution are often “clustered in particular communities,” said Darya Minovi, a senior analyst with the Union of Concerned Scientists, a nonprofit that advocates for environmental justice. When it comes to sterilizing facilities that emit ethylene oxide, areas inhabited largely by Black, Hispanic, low-income, and non-English-speaking people are disproportionately exposed, the group has found. Four sites that the EPA labeled high-risk are in low-income areas of Puerto Rico. Seven sterilizer plants operate in that U.S. territory. The EPA, responding to public concerns and to deepened scientific understanding of the hazards of ethylene oxide, recently released rules that the agency said would greatly reduce emissions of the toxic gas from sterilizing facilities. KeShaun Pearson, who was born and raised in south Memphis and has been active in fighting environmental threats, said he is frustrated that companies with dangerous emissions are allowed to create “toxic soup” in minority communities. In the area where the sterilization plant is located, 87% of the residents are people of color, and, according to the Southern Environmental Law Center, life expectancy there is about 10 years lower than the average for the county and state. The population within 5 miles of the sterilizer plant is mostly low-income, according to the Union of Concerned Scientists. Pearson was part of Memphis Community Against the Pipeline, a group formed in 2020 to stop a crude oil pipeline that would have run through Boxtown, a neighborhood established by emancipated slaves and freedmen after the signing of the Emancipation Proclamation of 1863. That campaign, which received public support from former Vice President Al Gore and actress-activist Jane Fonda, succeeded. After the ethylene oxide danger surfaced in 2022, the group changed the last word of its name from “pipeline” to “pollution.” Besides breast and lymphoid cancers, animal studies have linked inhaling the gas to tumors of the brain, lungs, connective tissue, uterus, and mammary glands. Last year, with the help of the Southern Environmental Law Center, the south Memphis community group urged the Shelby County Health Department to declare the ethylene oxide situation a public health emergency and shut down the sterilizing plant. But the health department said the company had complied with its existing air permit and with the EPA’s rules and regulations. A health department spokesperson, Joan Carr, said Shelby County enforces EPA regulations to ensure that companies comply with the federal Clean Air Act and that the agency has five air monitoring stations around the county to detect levels of other pollutants. When the county and the Tennessee Department of Health did a cancer cluster study in 2023, the agencies found no evidence of the clustering of high rates of leukemia, non-Hodgkin lymphoma, or breast or stomach cancer near the facility. There were “hot and cold spots” of breast cancer found, but the study said it could not conclude that the clusters were linked to the facility. Scientists have criticized the study’s methodology, saying it did not follow the Centers for Disease Control and Prevention’s recommendations for designing a cancer cluster investigation. Meanwhile, several people have sued the sterilizing company, claiming their health has been affected by the ethylene oxide emissions. In a lawsuit seeking class-action status, Reginaé Kendrick, 21, said she was diagnosed with a brain tumor at age 6. Chemotherapy and radiation have stunted her growth, destroyed her hair follicles, and prevented her from going through puberty, said her mother, Robbie Kendrick. In response to proposed stricter EPA regulations, meanwhile, the Tennessee attorney general helped lead 19 other state AGs in urging the agency to “forgo or defer regulating the use of EtO by commercial sterilizers.” Sims said she’s glad her neighborhood will have one less thing to worry about once Sterilization Services departs. But her feelings about the closure remain tempered. “Hope they don’t go to another residential area,” she said. KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about KFF. USE OUR CONTENTThis story can be republished for free (details). from https://ift.tt/wRZxuYW Check out http://plush-draw15.tumblr.com/ Cass Smith-Collins jumped through hoops to get the surgery that would match his chest to his gender. Living in Las Vegas and then 50, he finally felt safe enough to come out as a transgender man. He had his wife’s support and a doctor’s letter showing he had a long history of gender dysphoria, the psychological distress felt when one’s sex assigned at birth and gender identity don’t match. Although in-network providers were available, Smith-Collins selected Florida-based surgeon Charles Garramone, who markets himself as an early developer of female-to-male top surgery and says that he does not contract with insurance. Smith-Collins said he was willing to pay more to go out-of-network. “I had one shot to get the chest that I should have been born with, and I wasn’t going to chance it to someone who was not an expert at his craft,” he said. Smith-Collins arranged to spend a week in Florida and contacted friends there who could help him recover from the outpatient procedure, he said. Garramone’s practice required that the patient agree to its financial policies, according to documents shared by Smith-Collins. One document stated that “full payment” of Garramone’s surgical fees is required four weeks in advance of surgery and that all payments to the practice are “non-refundable.” Smith-Collins said he and his wife dipped into their retirement savings to cover the approximately $14,000 upfront. With prior authorization from his insurer in hand saying the procedure would be “covered,” he thought his insurance would reimburse anything he paid beyond his out-of-pocket maximum for out-of-network care: $6,900. The day before surgery, Smith-Collins signed another agreement from the surgeon’s practice, outlining how it would file an out-of-network claim with his insurance. Any insurance payment would be received by the doctor, it said. The procedure went well. Smith-Collins went home happy and relieved. Then the bill came. Or in this case: The reimbursement didn’t. The Patient: Cass Smith-Collins, now 52, who has employer-based coverage through UnitedHealthcare. Medical Services: Double-incision top surgery with nipple grafts, plus lab work. Service Provider: Aesthetic Plastic Surgery Institute, doing business as The Garramone Center, which is owned by Garramone, according to Florida public records. Total Bill: The surgeon’s practice billed the patient and insurance a total of $120,987 for his work. It charged the patient about $14,000 upfront — which included $300 for lab work and a $1,000 reservation fee — and then billed the patient’s insurer an additional $106,687. The surgeon later wrote the patient that the upfront fee was for the “cosmetic” portion of the surgery, while the insurance charge was for the “reconstructive” part. Initially, the insurer paid $2,193.54 toward the surgeon’s claim, and the patient received no reimbursement. After KFF Health News began reporting this story, the insurer reprocessed the surgeon’s claim and increased its payment to the practice to $97,738.46. Smith-Collins then received a reimbursement from Garramone of $7,245. What Gives: Many patients write to Bill of the Month each year with their own tangled billing question. In many cases — including this one — the short answer is that the patient misunderstood their insurance coverage. Smith-Collins was in a confusing situation. UnitedHealthcare said his out-of-network surgery would be “covered,” then it later told Smith-Collins it didn’t owe the reimbursement he had counted on. Then, after KFF Health News began reporting, he received a reimbursement. Adding to the confusion were the practice’s financial polices, which set a pre-surgery payment deadline, gave the doctor control of any insurance payment, and left the patient vulnerable to more bills (though, fortunately, he received none). Agreeing to an out-of-network provider’s own financial policy — which generally protects its ability to get paid and may be littered with confusing insurance and legal jargon — can create a binding contract that leaves a patient owing. In short, it can put the doctor in the driver’s seat, steering the money. The agreement Smith-Collins signed the day before surgery says that the patient understands he is receiving out-of-network care and “may be responsible for additional costs for all services provided” by the out-of-network practice. 
Federal billing protections shield patients from big, out-of-network bills — but not in cases in which the patient knowingly chose out-of-network care. Smith-Collins could have been on the hook for the difference between what his out-of-network doctor and insurer said the procedure should cost: nearly $102,000. Emails show Smith-Collins had a couple of weeks to review a version of the practice’s out-of-network agreement before he signed it. But he said he likely hadn’t read the entire document because he was focused on his surgery and willing to agree to just about anything to get it. “Surgery is an emotional experience for anyone, and that’s not an ideal time for anyone to sign a complex legal agreement,” said Marianne Udow-Phillips, a health policy instructor at the University of Michigan School of Public Health. Udow-Phillips, who reviewed the agreement, said it includes complicated terms that could confuse consumers. Another provision in the agreement says the surgeon’s upfront charges are “a separate fee that is not related to charges made to your insurance.” Months after his procedure, having received no reimbursement, Smith-Collins contacted his surgeon, he said. Garramone replied to him in an email, explaining that UnitedHealthcare had paid for the “reconstructive aspect of the surgery” — while the thousands of dollars Smith-Collins paid upfront was for the “cosmetic portion.” Filing an insurance claim had initially led to a payment for Garramone, but no refund for Smith-Collins. Garramone did not respond to questions from KFF Health News for this article or to repeated requests for an interview. Smith-Collins had miscalculated how much his insurance would pay for an out-of-network surgeon. Documents show that before the procedure Smith-Collins received a receipt from Garramone’s practice marked “final payment” with a zero balance due, as well as prior authorization from UnitedHealthcare stating that the surgery performed by Garramone would be “covered.” More from Bill of the Month
But out-of-network providers aren’t limited in what they can charge, and insurers don’t have a minimum they must pay. An explanation of benefits, or EOB, statement shows Garramone submitted a claim to UnitedHealthcare for more than $106,000. Of that, UnitedHealthcare determined the maximum it would pay — known as the “allowed amount” — was about $4,400. A UnitedHealthcare representative later told Smith-Collins in an email that the total was based on what Medicare would have paid for the procedure. Smith-Collins’ upfront charges of roughly $14,000 went well beyond the price the insurer deemed fair, and UnitedHealthcare wasn’t going to pay the difference. By UnitedHealthcare’s math, Smith-Collins’ share of its allowed amount was about $2,200, which is what counted toward his out-of-pocket costs. That meant, in the insurer’s eyes, Smith-Collins still hadn’t reached his $6,900 maximum for the year, so no refund. Neither UnitedHealthcare nor the surgeon provided KFF Health News with billing codes, making it difficult to compare the surgeon’s charges to cost estimates for the procedure. Garramone’s website says his fee varies depending on the size and difficulty of the procedure. The site says his prices reflect his experience and adds that “cheaper” may lead to “very poor results.” Though he spent more than he expected, Smith-Collins said he’ll never regret the procedure. He said he had lived with thoughts of suicide since youth, having realized at a young age that his body didn’t match his identity and feared others would target him for being trans. “It was a lifesaving thing,” he said. “I jumped through whatever hoops they wanted me to go through so I could get that surgery, so that I could finally be who I was.” 
The Resolution: Smith-Collins submitted two appeals with his insurer, asking UnitedHealthcare to reimburse him for what he spent beyond his out-of-pocket maximum. The insurer denied both appeals, finding its payments were correct based on the terms of his plan, and said his case was not eligible for a third, outside review. But after being contacted by KFF Health News, UnitedHealthcare reprocessed Garramone’s roughly $106,000 claim and increased its payment to the practice to $97,738.46. Maria Gordon Shydlo, a UnitedHealthcare spokesperson, told KFF Health News the company’s initial determination was correct, but that it had reprocessed the claim so that Smith-Collins is “only” responsible for his patient share: $6,755. “We are disappointed that this non-contracted provider elected to charge the member so much,” she said. After that new payment, Garramone gave Smith-Collins a $7,245 refund in mid-April. The Takeaway: Udow-Phillips, who worked in health insurance for decades and led provider services for Blue Cross Blue Shield of Michigan, said she had never seen a provider agreement like the one Smith-Collins signed. Patients should consult a lawyer before signing any out-of-network agreements, she said, and they should make sure they understand prior authorization letters from insurers. The prior authorization Smith-Collins received “doesn’t say covered in full, and it doesn’t say covered at what rate,” Udow-Phillips said, adding later, “I am sure [Smith-Collins] thought the prior authorization was for the cost of the procedure.” Patients can seek in-network care to feel more secure about what insurance will cover and what their doctors might charge. But for those who have a specific out-of-network doctor in mind, there are ways to try to avoid sticker shock, said Sabrina Corlette, a research professor and co-director of the Center on Health Insurance Reforms at Georgetown University:
Bill of the Month is a crowdsourced investigation by KFF Health News and NPR that dissects and explains medical bills. Do you have an interesting medical bill you want to share with us? Tell us about it! KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about KFF. USE OUR CONTENTThis story can be republished for free (details). from https://ift.tt/Ozl4Xwg Check out http://plush-draw15.tumblr.com/ |
 RSS Feed
RSS Feed
