The HostPublic health officials are watching with concern since a strain of bird flu spread to dairy cows in at least nine states, and to at least one dairy worker. But in the wake of covid-19, many farmers are loath to let in health authorities for testing. Meanwhile, another large health company — the Catholic hospital chain Ascension — has been targeted by a cyberattack, leading to serious problems at some facilities. This week’s panelists are Julie Rovner of KFF Health News, Rachel Cohrs Zhang of Stat, Alice Miranda Ollstein of Politico, and Sandhya Raman of CQ Roll Call. PanelistsAmong the takeaways from this week’s episode:
Also this week, Rovner interviews Atul Grover of the Association of American Medical Colleges about its recent analysis showing that graduating medical students are avoiding training in states with abortion bans and major restrictions. Plus, for “extra credit,” the panelists suggest health policy stories they read this week that they think you should read, too: Julie Rovner: NPR’s “Why Writing by Hand Beats Typing for Thinking and Learning,” by Jonathan Lambert. Alice Miranda Ollstein: Time’s “‘I Don’t Have Faith in Doctors Anymore.’ Women Say They Were Pressured Into Long-Term Birth Control,” by Alana Semuels. Rachel Cohrs Zhang: Stat’s “After Decades Fighting Big Tobacco, Cliff Douglas Now Leads a Foundation Funded by His Former Adversaries,” by Nicholas Florko. Sandhya Raman: The Baltimore Banner’s “People With Severe Mental Illness Are Stuck in Jail. Montgomery County Is the Epicenter of the Problem,” by Ben Conarck. Also mentioned on this week’s podcast:
CreditsFrancis Ying Audio producer Emmarie Huetteman EditorTo hear all our podcasts, click here. And subscribe to KFF Health News’ “What the Health?” on Spotify, Apple Podcasts, Pocket Casts, or wherever you listen to podcasts. KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about KFF. USE OUR CONTENTThis story can be republished for free (details). from https://ift.tt/tz9OE8L Check out http://plush-draw15.tumblr.com/
0 Comments
TURLOCK, Calif. — For much of his young life, Jorge Sanchez regularly gasped for air, at times coughing so violently that he’d almost throw up. His mother whisked him to the emergency room late at night and slept with him to make sure he didn’t stop breathing. “He’s had these problems since he was born, and I couldn’t figure out what was triggering his asthma,” Fabiola Sandoval said of her son, Jorge, now 4. “It’s so hard when your child is hurting. I was willing to try anything.” In January, community health workers visited Sandoval’s home in Turlock, a city in California’s Central Valley where dust from fruit and nut orchards billows through the air. They scoured Sandoval’s home for hazards and explained that harsh cleaning products, air fresheners, and airborne dust and pesticides can trigger an asthma attack. The team also provided Sandoval with air purifiers, a special vacuum cleaner that can suck dust out of the air, hypoallergenic mattress covers, and a humidity sensor — goods that retail for hundreds of dollars. Within a few months, Jorge was breathing easier and was able to run and play outside. 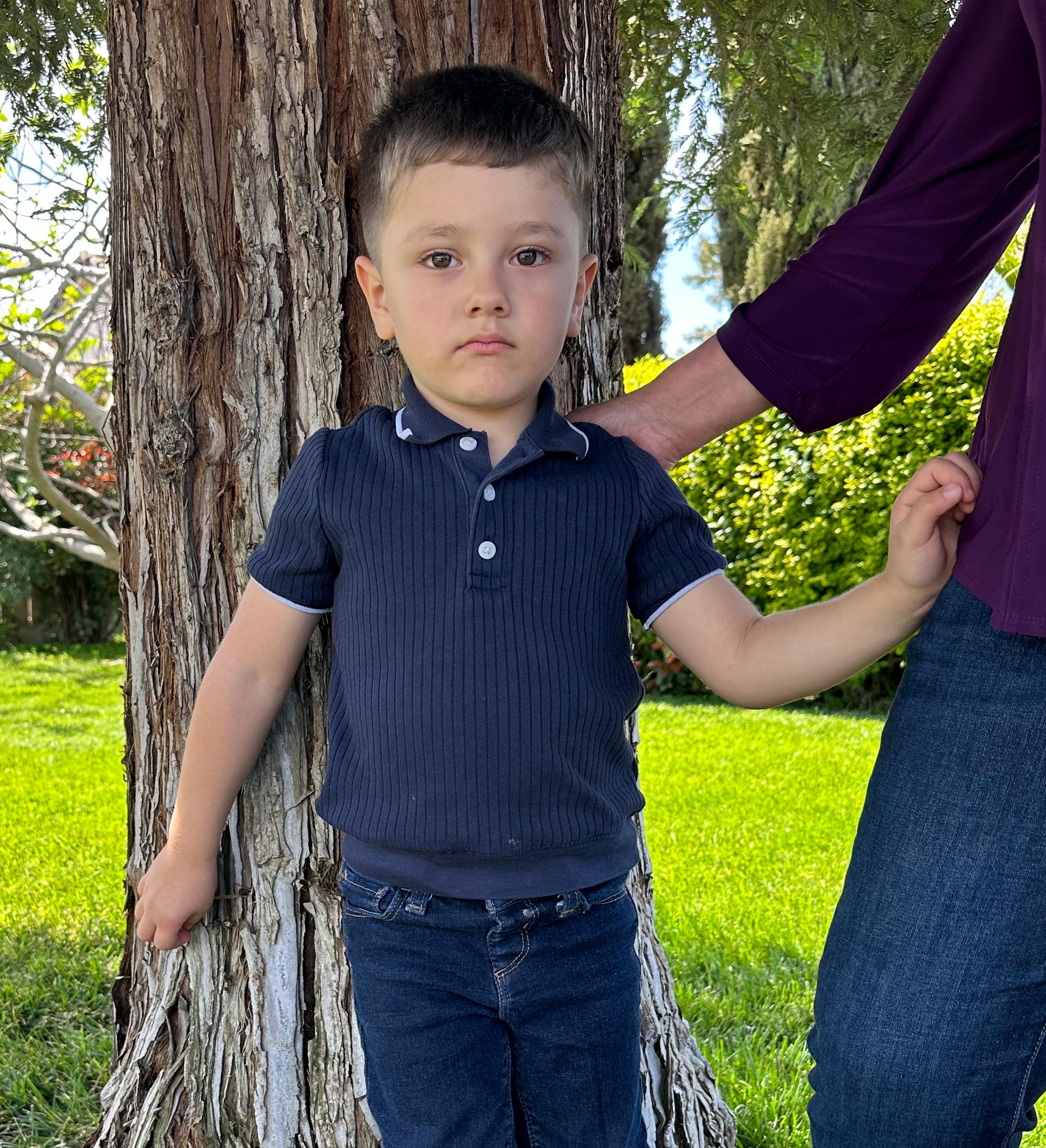
The in-home consultation and supplies were paid for by Medi-Cal, California’s Medicaid health insurance program for low-income residents. Gov. Gavin Newsom is spearheading an ambitious $12 billion experiment to transform Medi-Cal into both a health insurer and a social services provider, one that relies not only on doctors and nurses, but also community health workers and nonprofit groups that offer dozens of services, including delivering healthy meals and helping homeless people pay for housing. These groups are redefining health care in California as they compete with businesses for a share of the money, and become a new arm of the sprawling Medi-Cal bureaucracy that serves nearly 15 million low-income residents on an annual budget of $158 billion. But worker shortages, negotiations with health insurance companies, and learning to navigate complex billing and technology systems have hamstrung the community groups’ ability to deliver the new services: Now into the third year of the ambitious five-year experiment, only a small fraction of eligible patients have received benefits. “This is still so new, and everyone is just overwhelmed at this point, so it’s slow-going,” said Kevin Hamilton, a senior director at the Central California Asthma Collaborative. 
The collaborative has served about 3,650 patients, including Sandoval, in eight counties since early 2022, he said. It has years of experience with Medi-Cal patients in the Central Valley and has received about $1.5 million of the new initiative’s money. By contrast, CalOptima Health, Orange County’s primary Medi-Cal insurer, is new to offering asthma benefits and has signed up 58 patients so far. “Asthma services are so difficult to get going” because the nonprofit infrastructure for these services is virtually nonexistent, said Kelly Bruno-Nelson, CalOptima’s executive director for Medi-Cal. “We need more community-based organizations on board because they’re the ones who can serve a population that nobody wants to deal with.” Newsom, a Democrat in his second term, says his signature health care initiative, known as CalAIM, seeks to reduce the cost of caring for the state’s sickest and most vulnerable patients, including homeless Californians, foster children, former inmates, and people battling addiction disorders. In addition to in-home asthma remediation, CalAIM offers 13 broad categories of social services, plus a benefit connecting eligible patients with one-on-one care managers to help them obtain anything they need to get healthier, from grocery shopping to finding a job. The 25 managed-care insurance companies participating in Medi-Cal can choose which services they offer, and contract with community groups to provide them. Insurers have hammered out about 4,300 large and small contracts with nonprofits and businesses. So far, about 103,000 Medi-Cal patients have received CalAIM services and roughly 160,000 have been assigned personal care managers, according to state data, a sliver of the hundreds of thousands of patients who likely qualify. “We’re all new to health care, and a lot of this is such a foreign concept,” said Helena Lopez, executive director of A Greater Hope, a nonprofit organization providing social services in Riverside and San Bernardino counties, such as handing out baseball cleats to children to help them be active. Tiffany Sickler runs Koinonia Family Services, which offers California foster children mental health and other types of care, and even helped a patient pay off parking tickets. But the program is struggling on a shoestring budget. “If you want to do this, you have to learn all these new systems. It’s been a huge learning curve, and very time-consuming and frustrating, especially without adequate funding,” she said.  
Brandon Richards, a Newsom spokesperson, defended CalAIM, saying that it was “on the cutting edge of health care” and that the state was working to increase “awareness of these new services and support.” For nonprofits and businesses, CalAIM is a money-making opportunity — one that top state health officials hope to make permanent. Health insurers, which receive hefty payments from the state to serve more people and offer new services, share a portion with service providers. In some places, community groups are competing with national corporations for the new funding, such as Mom’s Meals, an Iowa-based company that delivers prepared meals across the United States. Mom’s Meals has an advantage over neighborhood nonprofit groups because it has long served seniors on Medicare and was able to immediately start offering the CalAIM benefit of home-delivered meals for patients with chronic diseases. But even Mom’s Meals isn’t reaching everyone who qualifies, because doctors and patients don’t always know it’s an option, said Catherine Macpherson, the company’s chief nutrition officer. “Utilization is not as high as it should be yet,” she said. “But we were well positioned, because we already had departments to do billing and contracting with health care.” Middleman companies also have their eye on the billions of CalAIM dollars and are popping up to assist small organizations to go up against established ones like Mom’s Meals. For instance, the New York-based Nonprofit Finance Fund is advising homeless service providers how to get more contracts and expand benefits. Full Circle Health Network, with 70 member organizations, is helping smaller nonprofit groups develop and deliver services primarily for families and foster children. Full Circle has signed a deal with Kaiser Permanente, allowing the health care giant to access its network of community groups. “We’re allowing organizations to launch these benefits much faster than they’ve been able to do and to reach more vulnerable people,” said Camille Schraeder, chief executive of Full Circle. “Many of these are grassroots organizations that have the trust and expertise on the ground, but they’re new to health care.” One of the biggest challenges community groups face is hiring workers, who are key to finding eligible patients and persuading them to participate. Kathryn Phillips, a workforce expert at the California Health Care Foundation, said there isn’t enough seed money for community groups to hire workers and pay for new technology platforms. “They bring the trust that is needed, the cultural competency, the diversity of languages,” she said. “But there needs to be more funding and reimbursement to build this workforce.” Health insurers say they are trying to increase the workforce. For instance, L.A. Care Health Plan, the largest Medi-Cal insurer in California, has given $66 million to community organizations for hiring and other CalAIM needs, said Sameer Amin, the group’s chief medical officer. “They don’t have the staffing to do all this stuff, so we’re helping with that all while teaching them how to build up their health care infrastructure,” he said. “Everyone wants a win, but this isn’t going to be successful overnight.” 
In the Central Valley, Jorge Sanchez is one of the lucky early beneficiaries of CalAIM. His mother credits the trust she established with community health workers, who spent many hours over multiple visits to teach her how to control her son’s asthma. “I used to love cleaning with bleach” but learned it can trigger breathing problems, Sandoval said. Since she implemented the health workers’ recommendations, Sandoval has been able to let Jorge sleep alone at night for the first time in four years. “Having this program and all the things available is amazing,” said Sandoval, as she pointed to the dirty dust cup in her new vacuum cleaner. “Now my son doesn’t have as many asthma attacks and he can run around and be a normal kid.” This article was produced by KFF Health News, which publishes California Healthline, an editorially independent service of the California Health Care Foundation. KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about KFF. USE OUR CONTENTThis story can be republished for free (details). from https://ift.tt/eAK3bWB Check out http://plush-draw15.tumblr.com/ Montana health officials have started a voucher system to help people with substance use disorders move into transitional housing as they rebuild their lives. But those who run the clinical houses said the new money isn’t enough to fix a financial hole after a prior state revamp. Residential treatment facilities are usually nondescript homes tucked into neighborhoods. The state’s lowest-intensity homes can provide people with alcohol and drug addiction leaving inpatient care a bridge to independent living. They’re the final option of four tiers of clinical housing and aim to offer residents stability amid daily stressors. But these particular houses have been disappearing — down to 10 sites today from 14 in 2022. That was the year the state started paying providers a blanket rate for their services through Medicaid, the state-federal program for people with low incomes and disabilities. At the same time, the state increased the homes’ staffing requirements. State health department officials lauded the 2022 change as an expansion in access to care, saying it increased the houses’ pay and matched the cost to operate. But providers warned at the time that it could backfire because the rates weren’t high enough to cover the new staffing rules. Terri Russell, who runs John “Scott” Hannon House, a treatment home in Helena, said it has been hard to break even since, and she’s watched other sites close under financial pressure. “It’s the hardest thing in the world to watch a person leave treatment and go back down to the homeless shelter, or go on the street,” Russell said. The new voucher program could help fill in some of the gap, Russell said. Approved by the state in April, it pays low-intensity treatment residences to house uninsured people as they sign up for Medicaid or other health coverage. The idea is to reduce barriers to care for vulnerable patients at a key point in their recovery. But the money is capped at $35 a day, with a $1,000 limit per resident a year. “It’s like it was somebody’s idea for a band-aid,” said Demetrius Fassas, who runs Butte Spirit Homes, which has two eight-bed facilities. He said the payments fall well below the cost of providing care. And, because of the vouchers’ cap, the aid could run out weeks before someone knows whether they qualify for Medicaid coverage. Low-intensity programs vary in how long patients stay; it could be a few months or more than a year. Fassas said when things go as intended, clients find stable jobs. That success can lead to residents earning too much money to qualify for Medicaid but not enough to afford the full cost of care. Providers have said funding issues are widespread for substance use disorder programs but that shortfalls especially hit these low-intensity homes. The tension in Montana mirrors challenges elsewhere around how to fund transitional treatment so that patients don’t fall off a cliff in their recovery because care is unavailable. As of 2022, at least 33 states were using money from Medicaid to help run residential treatment programs, KFF found. Federal rules prohibit Medicaid dollars from going to room and board at transitional homes, though states can chip in their own money. In North Dakota, for example, lawmakers set aside state funds for a voucher program that addresses treatment barriers, which include the cost of room and board. Montana once was among the states that let providers seek help covering room and board costs for its poorer residents. The money came from federal grants the state manages for addiction treatment and prevention. But those room and board grants stopped when Montana’s health department shifted to higher, bundled Medicaid rates in 2022. According to a state report last year, reducing the block grants to the low-intensity homes allowed officials to put that money toward other “prevention priorities.” The new rules the state added at the same time brought the residential facilities up to American Society of Addiction Medicine standards. That included having on-site clinical services, a clinical director for each home, and an employee working anytime a resident was in the home, including night shifts. Fassas, of Butte Spirit Homes, called the rules bittersweet. They increased the quality of care. But, Fassas said, he had to hire six additional workers to comply with the rules and the company now runs at a loss if he doesn’t find additional grants. Jon Ebelt, a spokesperson with the Montana Department of Public Health and Human Services, said the new rates, $143 a day per Medicaid resident, were developed by a state-paid contractor as part of Montana’s effort to match the cost of care. Ebelt said administrative costs were factored into the state’s Medicaid rate, and that traditional room and board expenses typically fall into that category. Low-intensity homes’ rates haven’t increased since they went into place in 2022. Malcolm Horn, chief behavioral health officer for the Rimrock Foundation, said the facilities need more help in covering expenses like the mortgage, repairs to the home, or feeding residents. The Rimrock Foundation, which is based in Billings, is one of Montana’s largest mental health providers. Horn said after the new rules were implemented, Rimrock converted one of its two low-intensity homes for women with children into high-intensity housing, which pays more. The switch displaced families in the low-intensity program. “We couldn’t actually sustain having both those houses,” Horn said. Montana officials set aside $300,000 for the voucher program and estimated that money would help cover initial housing for 329 people in 2024. Terri Todd, who runs the nonprofit Gratitude in Action in Billings for people in recovery, advocated for the program during the 2023 legislative session. She said the goal had been to follow North Dakota’s model to help cover addiction care for people facing barriers. But Montana lawmakers scaled that back, which Todd attributed to concerns about cost. Todd said that while what survived the legislature is less than what she had hoped for, the voucher program is still a start in addressing barriers to care. State Rep. Mike Yakawich, the Republican who proposed the program, said it was initially so broad, he learned, it overlapped with some existing efforts. But he said state staffers told him the low-intensity group homes’ room and board costs were an area that could use more funding. Yakawich said securing any money felt like a win in a funding tug-of-war. More help to stabilize the state’s mental health system is coming. Money for the vouchers is coming out of Republican Gov. Greg Gianforte’s HEART Fund initiative, which is due to invest about $25 million a year toward behavioral health programs. Separately, state officials recently announced that they’re creating grants to increase Montana’s bed capacity across residential facilities, including for substance use treatment providers. That money could go toward reopening closed facilities. But Yakawich said even that infusion of money won’t provide enough to go around. “Everybody wants a chunk of the pie, and not everyone’s going to get it,” he said. The voucher program is scheduled to expire in three years, Yakawich said. By then, he said, maybe he can persuade lawmakers to renew the program — with more money. KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about KFF. USE OUR CONTENTThis story can be republished for free (details). from https://ift.tt/kb4B3Er Check out http://plush-draw15.tumblr.com/ For help, call or text the National Maternal Mental Health Hotline at 1-833-TLC-MAMA (1-833-852-6262) or contact the 988 Suicide & Crisis Lifeline by dialing or texting “988.” Spanish-language services are also available. BRIDGEPORT, Conn. — Milagros Aquino was trying to find a new place to live and had been struggling to get used to new foods after she moved to Bridgeport from Peru with her husband and young son in 2023. When Aquino, now 31, got pregnant in May 2023, “instantly everything got so much worse than before,” she said. “I was so sad and lying in bed all day. I was really lost and just surviving.” Aquino has lots of company. Perinatal depression affects as many as 20% of women in the United States during pregnancy, the postpartum period, or both, according to studies. In some states, anxiety or depression afflicts nearly a quarter of new mothers or pregnant women. Many women in the U.S. go untreated because there is no widely deployed system to screen for mental illness in mothers, despite widespread recommendations to do so. Experts say the lack of screening has driven higher rates of mental illness, suicide, and drug overdoses that are now the leading causes of death in the first year after a woman gives birth. “This is a systemic issue, a medical issue, and a human rights issue,” said Lindsay R. Standeven, a perinatal psychiatrist and the clinical and education director of the Johns Hopkins Reproductive Mental Health Center. 
Standeven said the root causes of the problem include racial and socioeconomic disparities in maternal care and a lack of support systems for new mothers. She also pointed a finger at a shortage of mental health professionals, insufficient maternal mental health training for providers, and insufficient reimbursement for mental health services. Finally, Standeven said, the problem is exacerbated by the absence of national maternity leave policies, and the access to weapons. Those factors helped drive a 105% increase in postpartum depression from 2010 to 2021, according to the American Journal of Obstetrics & Gynecology. For Aquino, it wasn’t until the last weeks of her pregnancy, when she signed up for acupuncture to relieve her stress, that a social worker helped her get care through the Emme Coalition, which connects girls and women with financial help, mental health counseling services, and other resources. Mothers diagnosed with perinatal depression or anxiety during or after pregnancy are at about three times the risk of suicidal behavior and six times the risk of suicide compared with mothers without a mood disorder, according to recent U.S. and international studies in JAMA Network Open and The BMJ. The toll of the maternal mental health crisis is particularly acute in rural communities that have become maternity care deserts, as small hospitals close their labor and delivery units because of plummeting birth rates, or because of financial or staffing issues. This week, the Maternal Mental Health Task Force — co-led by the Office on Women’s Health and the Substance Abuse and Mental Health Services Administration and formed in September to respond to the problem — recommended creating maternity care centers that could serve as hubs of integrated care and birthing facilities by building upon the services and personnel already in communities. The task force will soon determine what portions of the plan will require congressional action and funding to implement and what will be “low-hanging fruit,” said Joy Burkhard, a member of the task force and the executive director of the nonprofit Policy Center for Maternal Mental Health. Burkhard said equitable access to care is essential. The task force recommended that federal officials identify areas where maternity centers should be placed based on data identifying the underserved. “Rural America,” she said, “is first and foremost.” There are shortages of care in “unlikely areas,” including Los Angeles County, where some maternity wards have recently closed, said Burkhard. Urban areas that are underserved would also be eligible to get the new centers. “All that mothers are asking for is maternity care that makes sense. Right now, none of that exists,” she said. Several pilot programs are designed to help struggling mothers by training and equipping midwives and doulas, people who provide guidance and support to the mothers of newborns. In Montana, rates of maternal depression before, during, and after pregnancy are higher than the national average. From 2017 to 2020, approximately 15% of mothers experienced postpartum depression and 27% experienced perinatal depression, according to the Montana Pregnancy Risk Assessment Monitoring System. The state had the sixth-highest maternal mortality rate in the country in 2019, when it received a federal grant to begin training doulas. To date, the program has trained 108 doulas, many of whom are Native American. Native Americans make up 6.6% of Montana’s population. Indigenous people, particularly those in rural areas, have twice the national rate of severe maternal morbidity and mortality compared with white women, according to a study in Obstetrics and Gynecology. Stephanie Fitch, grant manager at Montana Obstetrics & Maternal Support at Billings Clinic, said training doulas “has the potential to counter systemic barriers that disproportionately impact our tribal communities and improve overall community health.” Twelve states and Washington, D.C., have Medicaid coverage for doula care, according to the National Health Law Program. They are California, Florida, Maryland, Massachusetts, Michigan, Minnesota, Nevada, New Jersey, Oklahoma, Oregon, Rhode Island, and Virginia. Medicaid pays for about 41% of births in the U.S., according to the Centers for Disease Control and Prevention. Jacqueline Carrizo, a doula assigned to Aquino through the Emme Coalition, played an important role in Aquino’s recovery. Aquino said she couldn’t have imagined going through such a “dark time alone.” With Carrizo’s support, “I could make it,” she said. Genetic and environmental factors, or a past mental health disorder, can increase the risk of depression or anxiety during pregnancy. But mood disorders can happen to anyone. Teresa Martinez, 30, of Price, Utah, had struggled with anxiety and infertility for years before she conceived her first child. The joy and relief of giving birth to her son in 2012 were short-lived. Without warning, “a dark cloud came over me,” she said. Martinez was afraid to tell her husband. “As a woman, you feel so much pressure and you don’t want that stigma of not being a good mom,” she said. In recent years, programs around the country have started to help doctors recognize mothers’ mood disorders and learn how to help them before any harm is done. One of the most successful is the Massachusetts Child Psychiatry Access Program for Moms, which began a decade ago and has since spread to 29 states. The program, supported by federal and state funding, provides tools and training for physicians and other providers to screen and identify disorders, triage patients, and offer treatment options. But the expansion of maternal mental health programs is taking place amid sparse resources in much of rural America. Many programs across the country have run out of money. The federal task force proposed that Congress fund and create consultation programs similar to the one in Massachusetts, but not to replace the ones already in place, said Burkhard. In April, Missouri became the latest state to adopt the Massachusetts model. Women on Medicaid in Missouri are 10 times as likely to die within one year of pregnancy as those with private insurance. From 2018 through 2020, an average of 70 Missouri women died each year while pregnant or within one year of giving birth, according to state government statistics. Wendy Ell, executive director of the Maternal Health Access Project in Missouri, called her service a “lifesaving resource” that is free and easy to access for any health care provider in the state who sees patients in the perinatal period. About 50 health care providers have signed up for Ell’s program since it began. Within 30 minutes of a request, the providers can consult over the phone with one of three perinatal psychiatrists. But while the doctors can get help from the psychiatrists, mental health resources for patients are not as readily available. The task force called for federal funding to train more mental health providers and place them in high-need areas like Missouri. The task force also recommended training and certifying a more diverse workforce of community mental health workers, patient navigators, doulas, and peer support specialists in areas where they are most needed. A new voluntary curriculum in reproductive psychiatry is designed to help psychiatry residents, fellows, and mental health practitioners who may have little or no training or education about the management of psychiatric illness in the perinatal period. A small study found that the curriculum significantly improved psychiatrists’ ability to treat perinatal women with mental illness, said Standeven, who contributed to the training program and is one of the study’s authors. Nancy Byatt, a perinatal psychiatrist at the University of Massachusetts Chan School of Medicine who led the launch of the Massachusetts Child Psychiatry Access Program for Moms in 2014, said there is still a lot of work to do. “I think that the most important thing is that we have made a lot of progress and, in that sense, I am kind of hopeful,” Byatt said. Cheryl Platzman Weinstock’s reporting is supported by a grant from the National Institute for Health Care Management Foundation. KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about KFF. USE OUR CONTENTThis story can be republished for free (details). from https://ift.tt/fvYDMdt Check out http://plush-draw15.tumblr.com/ Inside the protesters’ encampment at UCLA, beneath the glow of hanging flashlights and a deafening backdrop of exploding flash-bangs, OB-GYN resident Elaine Chan suddenly felt like a battlefield medic.  related coverage from 2020 related coverage from 2020
Less-Lethal Weapons Blind, Maim and Kill. Victims Say Enough Is Enough.Read MorePolice were pushing into the camp after an hours-long standoff. Chan, 31, a medical tent volunteer, said protesters limped in with severe puncture wounds, but there was little hope of getting them to a hospital through the chaos outside. Chan suspects the injuries were caused by rubber bullets or other “less lethal” projectiles, which police have confirmed were fired at protesters. “It would pierce through skin and gouge deep into people’s bodies,” she said. “All of them were profusely bleeding. In OB-GYN we don’t treat rubber bullets. … I couldn’t believe that this was allowed to be [done to] civilians — students — without protective gear.” The UCLA protest, which gathered thousands in opposition to Israel’s ongoing bombing of Gaza, began in April and grew to a dangerous crescendo this month when counterprotesters and police clashed with the activists and their supporters. In interviews with KFF Health News, Chan and three other volunteer medics described treating protesters with bleeding wounds, head injuries, and suspected broken bones in a makeshift clinic cobbled together in tents with no electricity or running water. The medical tents were staffed day and night by a rotating team of doctors, nurses, medical students, EMTs, and volunteers with no formal medical training. At times, the escalating violence outside the tent isolated injured protesters from access to ambulances, the medics said, so the wounded walked to a nearby hospital or were carried beyond the borders of the protest so they could be driven to the emergency room. “I’ve never been in a setting where we’re blocked from getting higher level of care,” Chan said. “That was terrifying to me.”  
Three of the medics interviewed by KFF Health News said they were present when police swept the encampment May 2 and described multiple injuries that appeared to have been caused by “less lethal” projectiles. Less lethal projectiles — including beanbags filled with metal pellets, sponge-tipped rounds, and projectiles commonly known as rubber bullets — are used by police to subdue suspects or disperse crowds or protests. Police drew widespread condemnation for using the weapons against Black Lives Matter demonstrations that swept the country after the killing of George Floyd in 2020. Although the name of these weapons downplays their danger, less lethal projectiles can travel upward of 200 mph and have a documented potential to injure, maim, or kill. The medics’ interviews directly contradict an account from the Los Angeles Police Department. After police cleared the encampment, LAPD Chief Dominic Choi said in a post on the social platform X that there were “no serious injuries to officers or protestors” as police moved in and made more than 200 arrests. In response to questions from KFF Health News, both the LAPD and California Highway Patrol said in emailed statements that they would investigate how their officers responded to the protest. The LAPD statement said the agency was conducting a review of how it and other law enforcement agencies responded, which would lead to a “detailed report.” The Highway Patrol statement said officers warned the encampment that “non-lethal rounds” may be used if protesters did not disperse, and after some became an “immediate threat” by “launching objects and weapons,” some officers used “kinetic specialty rounds to protect themselves, other officers, and members of the public.” One officer received minor injuries, according to the statement. Video footage that circulated online after the protest appeared to show a Highway Patrol officer firing less lethal projectiles at protesters with a shotgun. “The use of force and any incident involving the use of a weapon by CHP personnel is a serious matter, and the CHP will conduct a fair and impartial investigation to ensure that actions were consistent with policy and the law,” the Highway Patrol said in its statement. The UCLA Police Department, which was also involved with the protest response, did not respond to requests for comment. Jack Fukushima, 28, a UCLA medical student and volunteer medic, said he witnessed a police officer shoot at least two protesters with less lethal projectiles, including a man who collapsed after being hit “square in the chest.” Fukushima said he and other medics escorted the stunned man to the medical tent then returned to the front lines to look for more injured. “It did really feel like a war,” Fukushima said. “To be met with such police brutality was so disheartening.” Back on the front line, police had breached the borders of the encampment and begun to scrum with protesters, Fukushima said. He said he saw the same officer who had fired earlier shoot another protester in the neck. The protester dropped to the ground. Fukushima assumed the worst and rushed to his side. “I find him, and I’m like, ‘Hey, are you OK?’” Fukushima said. “To the point of courage of these undergrads, he’s like, ‘Yeah, it’s not my first time.’ And then just jumps right back in.” Sonia Raghuram, 27, another medical student stationed in the tent, said that during the police sweep she tended to a protester with an open puncture wound on their back, another with a quarter-sized contusion in the center of their chest, and a third with a “gushing” cut over their right eye and possible broken rib. Raghuram said patients told her the wounds were caused by police projectiles, which she said matched the severity of their injuries. The patients made it clear the police officers were closing in on the medical tent, Raghuram said, but she stayed put. “We will never leave a patient,” she said, describing the mantra in the medical tent. “I don’t care if we get arrested. If I’m taking care of a patient, that’s the thing that comes first.” The UCLA protest is one of many that have been held on college campuses across the country as students opposed to Israel’s ongoing war in Gaza demand universities support a ceasefire or divest from companies tied to Israel. Police have used force to remove protesters at Columbia University, Emory University, and the universities of Arizona, Utah, and South Florida, among others. At UCLA, student protesters set up a tent encampment on April 25 in a grassy plaza outside the campus’s Royce Hall theater, eventually drawing thousands of supporters, according to the Los Angeles Times. Days later, a “violent mob” of counterprotesters “attacked the camp,” the Times reported, attempting to tear down barricades along its borders and throwing fireworks at the tents inside. The following night, police issued an unlawful assembly order, then swept the encampment in the early hours of May 2, clearing tents and arresting hundreds by dawn. Police have been widely criticized for not intervening as the clash between protesters and counterprotesters dragged on for hours. The University of California system announced it has hired an independent policing consultant to investigate the violence and “resolve unanswered questions about UCLA’s planning and protocols, as well as the mutual aid response.” Charlotte Austin, 34, a surgery resident, said that as counterprotesters were attacking she also saw about 10 private campus security officers stand by, “hands in their pockets,” as students were bashed and bloodied. Austin said she treated patients with cuts to the face and possible skull fractures. The medical tent sent at least 20 people to the hospital that evening, she said. “Any medical professional would describe these as serious injuries,” Austin said. “There were people who required hospitalization — not just a visit to the emergency room — but actual hospitalization.” 
Police Tactics ‘Lawful but Awful’ UCLA protesters are far from the first to be injured by less lethal projectiles. In recent years, police across the U.S. have repeatedly fired these weapons at protesters, with virtually no overarching standards governing their use or safety. Cities have spent millions to settle lawsuits from the injured. Some of the wounded have never been the same. During the nationwide protests following the police killing of George Floyd in 2020, at least 60 protesters sustained serious injuries — including blinding and a broken jaw — from being shot with these projectiles, sometimes in apparent violations of police department policies, according to a joint investigation by KFF Health News and USA Today. In 2004, in Boston, a college student celebrating a Red Sox victory was killed by a projectile filled with pepper-based irritant when it tore through her eye and into her brain. “They’re called less lethal for a reason,” said Jim Bueermann, a former police chief of Redlands, California, who now leads the Future Policing Institute. “They can kill you.” Bueermann, who reviewed video footage of the police response at UCLA at the request of KFF Health News, said the footage shows California Highway Patrol officers firing beanbag rounds from a shotgun. Bueermann said the footage did not provide enough context to determine if the projectiles were being used “reasonably,” which is a standard established by federal courts, or being fired “indiscriminately,” which was outlawed by a California law in 2021. “There is a saying in policing — ‘lawful but awful’ — meaning that it was reasonable under the legal standards but it looks terrible,” Bueermann said. “And I think a cop racking multiple rounds into a shotgun, firing into protesters, doesn’t look very good.” This article was produced by KFF Health News, which publishes California Healthline, an editorially independent service of the California Health Care Foundation. KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about KFF. USE OUR CONTENTThis story can be republished for free (details). from https://ift.tt/JX178x9 Check out http://plush-draw15.tumblr.com/ Ecstasy, “magic mushrooms” and other psychedelic drugs could soon be recognized as therapeutic in California — one of the latest states, and the biggest, to consider allowing their use as medicine. Legislation by state Sen. Scott Wiener (D) and Assembly member Marie Waldron (R) would allow the therapeutic use of psilocybin, mescaline, ecstasy and dimethyltryptamine — a chemical that occurs in the psychoactive ayahuasca plant mixture — in state-approved locations under the supervision of licensed individuals. It would also regulate the production, distribution, quality control and sale of those psychedelics. The bill is intended to get across the desk of Gov. Gavin Newsom, a Democrat who vetoed broader decriminalization legislation last year while calling psychedelics “an exciting frontier” and asking for “regulated treatment guidelines” in the next version. While most psychedelics are prohibited under federal law, research has shown them to be promising treatments for depression, anxiety, post-traumatic stress disorder and addiction. Several large cities including D.C., have effectively decriminalized their use, as has Colorado. Oregon, which previously decriminalized personal possession of all illegal drugs, including psychedelics, rolled back that policy but created a system to regulate the use of psilocybin mushrooms. Leanne Cavellini, 49, of Pleasanton, Calif., attended a psychedelic retreat in Mexico this year. She said the experience helped her overcome deep-rooted trauma. “The person I was before was a wound-up tight ball of rubber bands who kept everything in and felt a lot of fear and worry,” Cavellini said. “The person I am today is very free. I live in the present moment. I don’t live other people’s lives, and I don’t take on their emotions.” State regulation, though, doesn’t always mean easy access. Oregon permits consumption of psilocybin mushrooms only under the guidance of state-licensed facilitators in “psilocybin service centers.” Sessions can cost more than $2,500; they’re not covered by insurance. Colorado is building regulated “healing centers,” where people will be able to take psilocybin mushrooms and some other psychedelics under the supervision of licensed facilitators. In California, one obstacle is the state’s $45 billion budget deficit. Its elected leaders are already looking for programs to cut. One that doesn’t yet exist could be low-hanging fruit. Under the pending legislation, anyone hoping to be licensed to supervise people using psychedelics will need a professional health credential. Bills pending in several other states would ease access to psychedelics or relax current laws against them. Some first responder and veterans groups are among legalization’s biggest boosters, and there is significant public support. A survey out of the University of California at Berkeley last year showed 61 percent of registered voters in the United States support regulated therapeutic access to psychedelics — though nearly half of those respondents said such drugs were not “good for society.” Ken Finn, the former president of the American Board of Pain Medicine, said although the science around psychedelics is promising, the California legislation is premature “pending more robust and rigorous research to protect public safety.” This article is not available for syndication due to republishing restrictions. If you have questions about the availability of this or other content for republication, please contact [email protected]. KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about KFF. USE OUR CONTENTThis story can be republished for free (details). from https://ift.tt/vZKLjh8 Check out http://plush-draw15.tumblr.com/ ROCHESTER, N.Y. — Jolynn Mungenast spends her days looking for ways to help people pay their hospital bills. Working out of a warehouse-like building in a scruffy corner of this former industrial town, Mungenast gently walks patients through health insurance options, financial aid, and payment plans. Most want to pay, said Mungenast, a financial counselor at Rochester Regional Health. Very often, they simply can’t. “They’re scared. They’re nervous. They’re upset,” said Mungenast, who on one recent call worked with an older patient to settle a $143 bill. “They do think ‘I don’t want this to affect my credit rating. I don’t want you to come take my house.’” At Rochester Regional Health, that won’t happen. The nonprofit system in upstate New York is one of only a few nationally that bar all aggressive collection activities. Patients who don’t pay won’t be taken to court. Their wages won’t be garnished. They won’t end up with liens on their homes or be denied care. And unpaid bills won’t sink their credit scores. American hospital officials often insist that lawsuits and other aggressive collections, though unsavory, are necessary to protect health systems’ finances and deter freeloading. But at Rochester Regional, ditching these collection tactics hasn’t hurt the bottom line, said Jennifer Eslinger, chief operating officer. The system has even been able to move staff out of its collections department as it spends less to go after patients who haven’t paid. Eslinger said there’s been another benefit to the change: rebuilding trust with patients. “We think and talk a lot and strategize a lot about where is the distrust in health care,” she said. “We have to remove that as a barrier to meaningful health care. We have to get the trust with the populations that we serve so that they can get the care that they need.” ‘Folks Cannot Afford This’ Rochester Regional, a large health system serving a wide swath of communities along the south shore of Lake Ontario, is big, with more than $3 billion in annual revenue. But in a place where once-mighty employers like Kodak and Xerox have withered, finances can be challenging. In 2022, Rochester Regional finished nearly $200 million in the red. Patients have their own challenges. Unable to afford their bills, many ended up in collections, or even on the receiving end of lawsuits. “We would go to court,” acknowledged Lisa Poworoznek, head of financial counseling at Rochester Regional. Then, before the pandemic, hospital leaders looked more closely at why patients weren’t paying. The barriers became clear, Poworoznek said: confusing insurance plans, high deductibles, and inadequate savings. “There are so many different situations that patients have,” she said. “It’s really just not as simple as demanding payment and then filing legal action.” Nationally, nearly half of adults are unable to cover a $500 medical bill without going into debt, a 2022 KFF poll found. At the same time, the average annual deductible for a single worker with job-based coverage now tops $1,500. Instead of chasing people who didn’t pay — a costly process that often yields meager returns — Rochester Regional resolved to find ways to get patients to settle bills before collections started. The health system undertook new efforts to enroll people in health insurance. New York has among the most robust safety-net systems in the country. Rochester Regional also bolstered its financial assistance program, making it easier for low-income patients to access free or discounted care. At many hospitals, applying for aid is complicated — long applications that demand extensive information about patients’ income and assets, including cars, retirement accounts, and property, KFF Health News has found. Patients applying for aid at Rochester Regional are asked to disclose only their income. Finally, the health system looked for ways to get more people on payment plans so they could pay off big bills over a year or two. Importantly, the payment plans are interest-free. That was a change. Rochester Regional, like some other major health systems across the country such as Atrium Health, used to rely on financing companies that charged interest, which could add thousands of dollars to patients’ debts. “Folks cannot afford this,” Poworoznek said. Ending ‘Extraordinary Collection Actions’ 
Working more closely with patients on their bills allowed Rochester Regional to stop taking them to court. The health system also stopped reporting people to credit bureaus, a practice many medical providers use that can depress consumers’ credit scores, making it harder to rent an apartment, get a car loan, or even get a job. In 2020, Rochester Regional adopted a written policy barring all aggressive collections by the system or its contracted collection agencies. That put Rochester Regional in select company. A 2022 KFF Health News investigation of billing practices at 528 hospitals around the country found just 19 that explicitly prohibit what are called extraordinary collection actions. Among them are leading academic medical centers, including UCLA and Stanford University, but also community hospitals such as El Camino Hospital in California’s Bay Area and St. Anthony Community Hospital outside New York City. Also barring extraordinary collection actions: the University of Vermont Medical Center; Ochsner Health, a large New Orleans-based nonprofit; and UPMC, a mammoth system based in Pittsburgh. Like Rochester Regional, UPMC officials said they were able to scrap aggressive collections by developing better systems that allow patients to pay off their bills. Elisabeth Benjamin, a vice president at the Community Service Society of New York, a nonprofit that has led efforts to restrict aggressive hospital collections, said there’s no reason more hospitals shouldn’t follow suit, particularly nonprofits that are expected to serve their communities in exchange for their tax-exempt status. “The value is to promote health, to care about a population, to promote health equity,” Benjamin said. “Suing people for medical debt or engaging in extraordinary collection actions is really anathema to all those values,” she said. “Forget about your ‘cancer-mobile’ or your child vaccination clinic.” Rochester Regional’s approach doesn’t eliminate medical debt, which burdens an estimated 100 million people in the U.S. And payment plans like those the system encourages can still mean big sacrifices for some families. But Benjamin applauded Rochester Regional’s ban on aggressive collections. “I give them big props,” she said. “It never should have been allowed.” New laws in New York now prohibit all medical bills from being reported to credit bureaus and restrict other collection tactics, such as wage garnishments. Many hospital finance officials nevertheless say they need the option to pursue patients who have the means to pay. “Maybe it’s on a very specific case where there is an issue with someone just not paying their bill,” said Richard Gundling, a senior vice president at the Healthcare Financial Management Association, a trade group. But at Rochester Regional’s finance offices, officials say they almost never find patients who just refuse to pay. More often, the problem is the bills are simply too big. “People just don’t have $5,000 to pay off that bill,” Poworoznek said. On her calls with patients, Mungenast tries to reassure the patients on the other end of the line. “Put yourself in their shoes,” she said. “How would it be if that was you receiving that?” About This Project“Diagnosis: Debt” is a reporting partnership between KFF Health News and NPR exploring the scale, impact, and causes of medical debt in America. The series draws on original polling by KFF, court records, federal data on hospital finances, contracts obtained through public records requests, data on international health systems, and a yearlong investigation into the financial assistance and collection policies of more than 500 hospitals across the country. Additional research was conducted by the Urban Institute, which analyzed credit bureau and other demographic data on poverty, race, and health status for KFF Health News to explore where medical debt is concentrated in the U.S. and what factors are associated with high debt levels. The JPMorgan Chase Institute analyzed records from a sampling of Chase credit card holders to look at how customers’ balances may be affected by major medical expenses. And the CED Project, a Denver nonprofit, worked with KFF Health News on a survey of its clients to explore links between medical debt and housing instability. KFF Health News journalists worked with KFF public opinion researchers to design and analyze the “KFF Health Care Debt Survey.” The survey was conducted Feb. 25 through March 20, 2022, online and via telephone, in English and Spanish, among a nationally representative sample of 2,375 U.S. adults, including 1,292 adults with current health care debt and 382 adults who had health care debt in the past five years. The margin of sampling error is plus or minus 3 percentage points for the full sample and 3 percentage points for those with current debt. For results based on subgroups, the margin of sampling error may be higher. Reporters from KFF Health News and NPR also conducted hundreds of interviews with patients across the country; spoke with physicians, health industry leaders, consumer advocates, debt lawyers, and researchers; and reviewed scores of studies and surveys about medical debt. KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about KFF. USE OUR CONTENTThis story can be republished for free (details). from https://ift.tt/KlRcfSh Check out http://plush-draw15.tumblr.com/   
PRESQUE ISLE, Maine — Outside the Mi’kmaq Nation’s health department sits a dome-shaped tent, built by hand from saplings and covered in black canvas. It’s one of several sweat lodges on the tribe’s land, but this one is dedicated to helping people recover from addiction. Up to 10 people enter the lodge at once. Fire-heated stones — called grandmothers and grandfathers, for the spirits they represent — are brought inside. Water is splashed on the stones, and the lodge fills with steam. It feels like a sauna, but hotter. The air is thicker, and it’s dark. People pray and sing songs. When they leave the lodge, it is said, they reemerge from the mother’s womb. Cleansed. Reborn. The experience can be “a vital tool” in healing, said Katie Espling, health director for the roughly 2,000-member tribe. She said patients in recovery have requested sweat lodges for years as a cultural element to complement the counseling and medications the tribe’s health department already provides. But insurance doesn’t cover sweat ceremonies, so, until now, the department couldn’t afford to provide them. In the past year, the Mi’kmaq Nation received more than $150,000 from settlements with companies that made or sold prescription painkillers and were accused of exacerbating the overdose crisis. A third of that money was spent on the sweat lodge. Health care companies are paying out more than $1.5 billion to hundreds of tribes over 15 years. This windfall is similar to settlements that many of the same companies are paying to state governments, which total about $50 billion. To some people, the lower payout for tribes corresponds to their smaller population. But some tribal citizens point out that the overdose crisis has had a disproportionate effect on their communities. Native Americans had the highest overdose death rates of any racial group each year from 2020 to 2022. And federal officials say those statistics were likely undercounted by about 34% because Native Americans’ race is often misclassified on death certificates. Still, many tribal leaders are grateful for the settlements and the unique way the money can be spent: Unlike the state payments, money sent to tribes can be used for traditional and cultural healing practices — anything from sweat lodges and smudging ceremonies to basketmaking and programs that teach tribal languages. “To have these dollars to do that, it’s really been a gift,” said Espling of the Mi'kmaq tribe. “This is going to absolutely be fundamental to our patients’ well-being” because connecting with their culture is “where they’ll really find the deepest healing.” Public health experts say the underlying cause of addiction in many tribal communities is intergenerational trauma, resulting from centuries of brutal treatment, including broken treaties, land theft, and a government-funded boarding school system that sought to erase the tribes’ languages and cultures. Along with a long-running lack of investment in the Indian Health Service, these factors have led to lower life expectancy and higher rates of addiction, suicide, and chronic diseases. Using settlement money to connect tribal citizens with their traditions and reinvigorate pride in their culture can be a powerful healing tool, said Andrea Medley, a researcher with the Johns Hopkins Center for Indigenous Health and a member of the Haida Nation. She helped create principles for how tribes can consider spending settlement money. Medley said that having respect for those traditional elements outlined explicitly in the settlements is “really groundbreaking.” ‘A Drop in the Bucket’ Of the 574 federally recognized tribes, more than 300 have received payments so far, totaling more than $371 million, according to Kevin Washburn, one of three court-appointed directors overseeing the tribal settlements. Although that sounds like a large sum, it pales in comparison with what the addiction crisis has cost tribes. There are also hundreds of tribes that are excluded from the payments because they aren’t federally recognized. “These abatement funds are like a drop in the bucket compared to what they’ve spent, compared to what they anticipate spending,” said Corey Hinton, a lawyer who represented several tribes in the opioid litigation and a citizen of the Passamaquoddy Tribe. “Abatement is a cheap term when we’re talking about a crisis that is still engulfing and devastating communities.” Even leaders of the Navajo Nation — the largest federally recognized tribe in the United States, which has received $63 million so far — said the settlements can’t match the magnitude of the crisis. “It’ll do a little dent, but it will only go so far,” said Kim Russell, executive director of the Navajo Department of Health. The Navajo Nation is trying to stretch the money by using it to improve its overall health system. Officials plan to use the payouts to hire more coding and billing employees for tribe-operated hospitals and clinics. Those workers would help ensure reimbursements keep flowing to the health systems and would help sustain and expand services, including addiction treatment and prevention, Russell said. Navajo leaders also want to hire more clinicians specializing in substance use treatment, as well as primary care doctors, nurses, and epidemiologists. “Building buildings is not what we want” from the opioid settlement funds, Russell said. “We’re nation-building.” High Stakes for Small Tribes Smaller nations like the Poarch Band of Creek Indians in southern Alabama are also strategizing to make settlement money go further. For the tribe of roughly 2,900 members, that has meant investing $500,000 — most of what it has received so far — into a statistical modeling platform that its creators say will simulate the opioid crisis, predict which programs will save the most lives, and help local officials decide the most effective use of future settlement cash. Some recovery advocates have questioned the model’s value, but the tribe’s vice chairman, Robert McGhee, said it would provide the data and evidence needed to choose among efforts competing for resources, such as recovery housing or peer support specialists. The tribe wants to do both, but realistically, it will have to prioritize. “If we can have this model and we put the necessary funds to it and have the support, it'll work for us,” McGhee said. “I just feel it in my gut.”  
The stakes are high. In smaller communities, each death affects the whole tribe, McGhee said. The loss of one leader marks decades of lost knowledge. The passing of a speaker means further erosion of the Native language. For Keesha Frye, who oversees the Poarch Band of Creek Indians’ tribal court and the sober living facility, using settlement money effectively is personal. “It means a lot to me to get this community well because this is where I live and this is where my family lives,” she said. Erik Lamoreau in Maine also brings personal ties to this work. More than a decade ago, he sold drugs on Mi’kmaq lands to support his own addiction. “I did harm in this community and it was really important for me to come back and try to right some of those wrongs,” Lamoreau said. Today, he works for the tribe as a peer recovery coordinator, a new role created with the opioid settlement funds. He uses his experience to connect with others and help them with recovery — whether that means giving someone a ride to court, working on their résumé, exercising together at the gym, or hosting a cribbage club, where people play the card game and socialize without alcohol or drugs. Beginning this month, Lamoreau’s work will also involve connecting clients who seek cultural elements of recovery to the new sweat lodge service — an effort he finds promising. “The more in tune you are with your culture — no matter what culture that is — it connects you to something bigger,” Lamoreau said. “And that’s really what we look at when we’re in recovery, when we talk about spiritual connection. It’s something bigger than you.” KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about KFF. USE OUR CONTENTThis story can be republished for free (details). from https://ift.tt/gzoV9mA Check out http://plush-draw15.tumblr.com/ LAKE ELSINORE, Calif. — Yahushua Robinson was an energetic boy who jumped and danced his way through life. Then, a physical education teacher instructed the 12-year-old to run outside on a day when the temperature climbed to 107 degrees. “We lose loved ones all the time, but he was taken in a horrific way,” his mother, Janee Robinson, said from the family’s Inland Empire home, about 80 miles southeast of Los Angeles. “I would never want nobody to go through what I’m going through.” The day her son died, Robinson, who teaches phys ed, kept her elementary school students inside, and she had hoped her children’s teachers would do the same. The Riverside County Coroner’s Bureau ruled that Yahushua died on Aug. 29 of a heart defect, with heat and physical exertion as contributing factors. His death at Canyon Lake Middle School came on the second day of an excessive heat warning, when people were advised to avoid strenuous activities and limit their time outdoors. Yahushua’s family is supporting a bill in California that would require the state Department of Education to create guidelines that govern physical activity at public schools during extreme weather, including setting threshold temperatures for when it’s too hot or too cold for students to exercise or play sports outside. If the measure becomes law, the guidelines will have to be in place by Jan. 1, 2026. 
Many states have adopted protocols to protect student athletes from extreme heat during practices. But the California bill is broader and would require educators to consider all students throughout the school day and in any extreme weather, whether they’re doing jumping jacks in fourth period or playing tag during recess. It’s unclear if the bill will clear a critical committee vote scheduled for May 16. “Yahushua’s story, it’s very touching. It’s very moving. I think it could have been prevented had we had the right safeguards in place,” said state Sen. Melissa Hurtado (D-Bakersfield), one of the bill’s authors. “Climate change is impacting everyone, but it’s especially impacting vulnerable communities, especially our children.” Last year marked the planet’s warmest on record, and extreme weather is becoming more frequent and severe, according to the National Oceanic and Atmospheric Administration. Even though most heat deaths and illnesses are preventable, about 1,220 people in the United States are killed by extreme heat every year, according to the Centers for Disease Control and Prevention. Young children are especially susceptible to heat illness because their bodies have more trouble regulating temperature, and they rely on adults to protect them from overheating. A person can go from feeling dizzy or experiencing a headache to passing out, having a seizure, or going into a coma, said Chad Vercio, a physician and the division chief of general pediatrics at Loma Linda University Health. “It can be a really dangerous thing,” Vercio said of heat illness. “It is something that we should take seriously and figure out what we can do to avoid that.” 
It’s unclear how many children have died at school from heat exposure. Eric Robinson, 15, had been sitting in his sports medicine class learning about heatstroke when his sister arrived at his high school unexpectedly the day their brother died. “They said, ‘OK, go home, Eric. Go home early.’ I walked to the car and my sister’s crying. I couldn’t believe it,” he said. “I can’t believe that my little brother’s gone. That I won’t be able to see him again. And he’d always bugged me, and I would say, ‘Leave me alone.’” That morning, Eric had done Yahushua’s hair and loaned him his hat and chain necklace to wear to school. As temperatures climbed into the 90s that morning, a physical education teacher instructed Yahushua to run on the blacktop. His friends told the family that the sixth grader had repeatedly asked the teacher for water but was denied, his parents said. The school district has refused to release video footage to the family showing the moment Yahushua collapsed on the blacktop. He died later that day at the hospital. Melissa Valdez, a Lake Elsinore Unified School District spokesperson, did not respond to calls seeking comment. 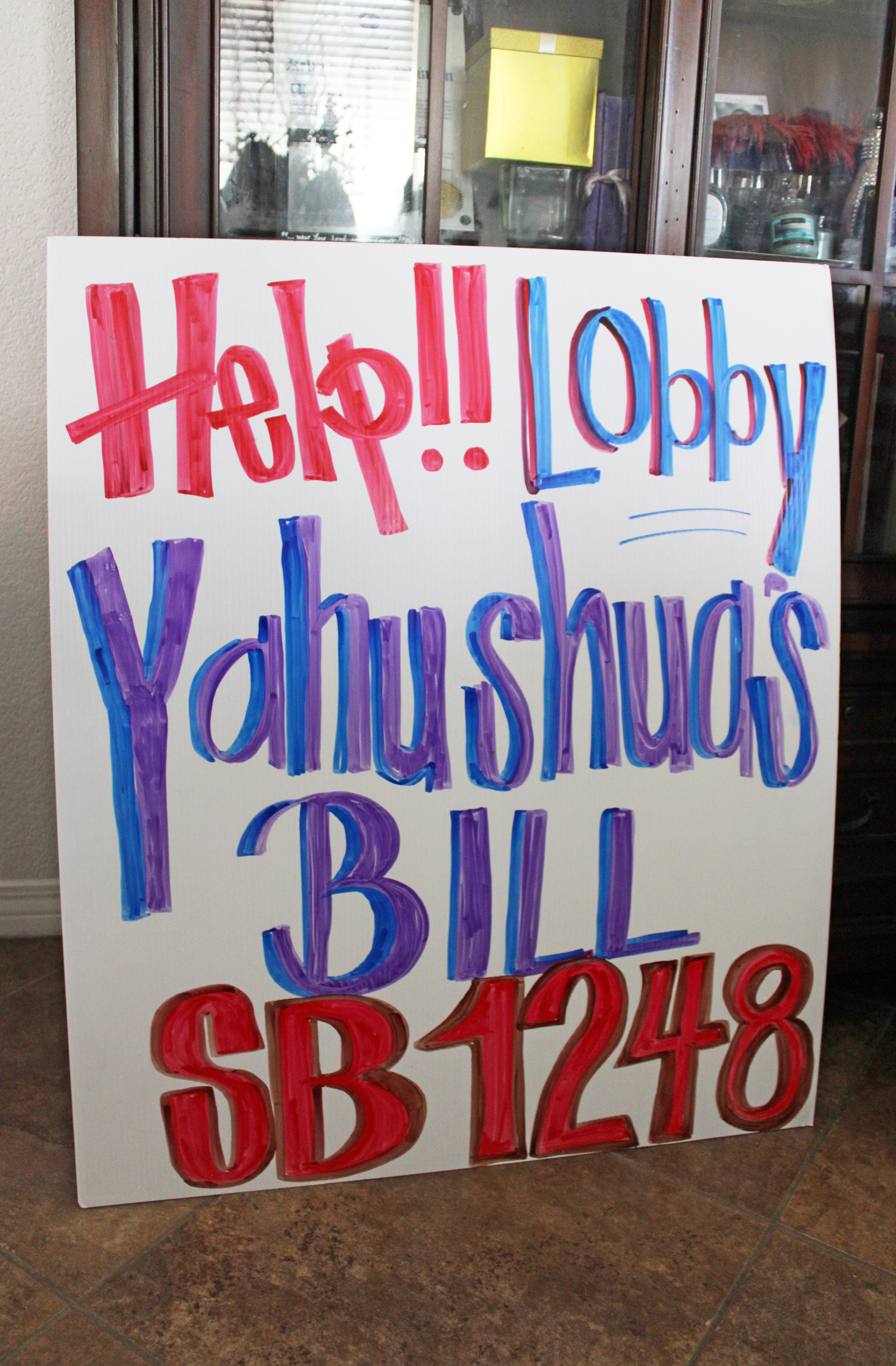
Schoolyards can reach dangerously high temperatures on hot days, with asphalt sizzling up to 145 degrees, according to findings by researchers at the UCLA Luskin Center for Innovation. Some school districts, such as San Diego Unified and Santa Ana Unified, have hot weather plans or guidelines that call for limiting physical activity and providing water to kids. But there are no statewide standards that K-12 schools must implement to protect students from heat illness. Under the bill, the California Department of Education must set temperature thresholds requiring schools to modify students’ physical activities during extreme weather, such as heat waves, wildfires, excessive rain, and flooding. Schools would also be required to come up with plans for alternative indoor activities, and staff must be trained to recognize and respond to weather-related distress. California has had heat rules on the books for outdoor workers since 2005, but it was a latecomer to protecting student athletes, according to the Korey Stringer Institute at the University of Connecticut, which is named after a Minnesota Vikings football player who died from heatstroke in 2001. By comparison, Florida, where Gov. Ron DeSantis, a Republican, this spring signed a law preventing cities and counties from creating their own heat protections for outdoor workers, has the best protections for student athletes, according to the institute. Douglas Casa, a professor of kinesiology and the chief executive officer of the institute, said state regulations can establish consistency about how to respond to heat distress and save lives. “The problem is that each high school doesn’t have a cardiologist and doesn’t have a thermal physiologist and doesn’t have a sickling expert,” Casa said of the medical specialties for heat illness. In 2022, California released an Extreme Action Heat Plan that recommended state agencies “explore implementation of indoor and outdoor heat exposure rules for schools,” but neither the administration of Gov. Gavin Newsom, a Democrat, nor lawmakers have adopted standards. Lawmakers last year failed to pass legislation that would have required schools to implement a heat plan and replace hot surfaces, such as cement and rubber, with lower-heat surfaces, such as grass and cool pavement. That bill, which drew opposition from school administrators, stalled in committee, in part over cost concerns. Naj Alikhan, a spokesperson for the Association of California School Administrators, said the new bill takes a different approach and would not require structural and physical changes to schools. The association has not taken a position on the measure, and no other organization has registered opposition. The Robinson family said children’s lives ought to outweigh any costs that might come with preparing schools to deal with the growing threat of extreme weather. Yahushua‘s death, they say, could save others. “I really miss him. I cry every day,” said Yahushua’s father, Eric Robinson. “There’s no one day that go by that I don’t cry about my boy.” 
This article was produced by KFF Health News, which publishes California Healthline, an editorially independent service of the California Health Care Foundation. KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about KFF. USE OUR CONTENTThis story can be republished for free (details). from https://ift.tt/6WsFUMo Check out http://plush-draw15.tumblr.com/ Facility fees are charges tacked on for visiting a doctor’s office or even a telehealth visit. They’re becoming increasingly common and they can add hundreds of dollars to your bill. “An Arm and a Leg” host Dan Weissmann wants to know how often this happens, where, and how much it costs patients. If you’ve ever seen a charge for a facility fee on your medical bill — especially for a visit or service that didn’t take place in a hospital — “An Arm and a Leg” wants to hear from you.Click here to share your story. It may be featured on an upcoming episode. Dan Weissmann @danweissmann Host and producer of "An Arm and a Leg." Previously, Dan was a staff reporter for Marketplace and Chicago's WBEZ. His work also appears on All Things Considered, Marketplace, the BBC, 99 Percent Invisible, and Reveal, from the Center for Investigative Reporting.CreditsEmily Pisacreta Producer Adam Raymonda Audio wizard Ellen Weiss Editor“An Arm and a Leg” is a co-production of KFF Health News and Public Road Productions. To keep in touch with “An Arm and a Leg,” subscribe to the newsletter. You can also follow the show on Facebook and the social platform X. And if you’ve got stories to tell about the health care system, the producers would love to hear from you. To hear all KFF Health News podcasts, click here. And subscribe to “An Arm and a Leg” on Spotify, Apple Podcasts, Pocket Casts, or wherever you listen to podcasts. KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about KFF. USE OUR CONTENTThis story can be republished for free (details). from https://ift.tt/P4msUZ1 Check out http://plush-draw15.tumblr.com/ |
 RSS Feed
RSS Feed
